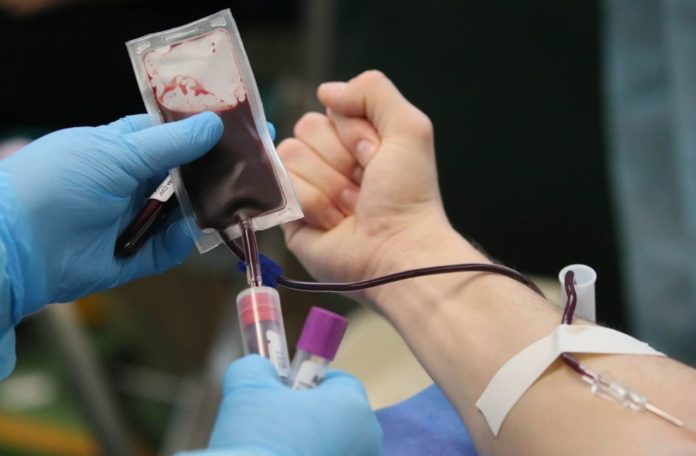
A new study shows that it’s possible to pass on the brain benefits that marathon-running mice get to their non-active peers.
Physical exercise is good for a mouse’s brain, as well as your own, because it makes it smarter. There have been a lot of studies done on mice, humans, and even lab glassware that show this. Now, a new study shows that it’s possible to pass on the brain benefits that marathon-running mice get to their couch potatoes.
Researchers at Stanford University School of Medicine discovered that blood from young adult mice who do a lot of exercise enhances the brains of the same-aged, sedentary mice. That effect appears to be mostly due to a single protein seen in the blood of exercising mice.
The discovery could pave the way for medicines that reduce the risk of neurodegenerative disease or halt its course by controlling brain inflammation in those who don’t get enough exercise.
The Stanford researchers examined blood samples from athletic and sedentary mice of the same age. They discovered that giving sedentary mice blood from running mice reduced neuroinflammation and increased cognitive performance. Furthermore, the scientists found a blood-borne protein that appears to be crucial in the anti-inflammatory exercise effect.
According to Tony Wyss-Coray, PhD, professor of neurology and neurological sciences, neuroinflammation has been closely linked to neurodegenerative diseases in humans and animal studies have shown that neuroinflammation causes neurodegenerative diseases and that reversing or lowering neuroinflammation can help people live longer.
“We’ve discovered that this exercise effect can be attributed to a large extent to factors in the blood, and we can transfer that effect to a same-aged, non-exercising individual,” added Wyss-Coray, the D. H. Chen Professor II.
For the study, the researchers placed either working or locked running wheels in the cages of 3-month-old lab mice, which have a metabolic age of 25 years. When marathoner mice were compared to inactive mice, a month of consistent running was enough to significantly increase the number of neurons and other cells in their brains.
The researchers next took blood samples from marathon runners and inactive mice as controls. They next injected plasma (the cell-free part of blood) from marathoner or couch-potato animals into additional inactive mice every three days. Each injection accounted for 7% to 8% of the total blood volume of the recipient mouse. (In humans, a comparable amount would be around ½ to ¾ of a pint.)
“The mice getting runner blood were smarter,” Wyss-Coray added.
Sedentary mice treated with marathoner plasma beat their equally sedentary friends that got couch-potato plasma in two memory tests.
Furthermore, sedentary mice given marathoner mice’s plasma had more cells that give rise to new neurons in the hippocampus (a brain region related to memory and navigation) than that given couch-potato plasma.
The researchers evaluated the levels of activation of hundreds of genes in the brain of sedentary animals given marathoner vs couch-potato plasma. The activation levels of the 250 genes whose activation levels changed the most in response to marathoner plasma were known to be most strongly associated with inflammatory processes, and their activation-level alterations showed decreased neuroinflammation in mice given marathoner blood transfusions.
“The runners’ blood was clearly doing something to the brain, even though it had been delivered outside the brain, systemically,” said Wyss-Coray.
When the Stanford team looked at the proteins in the marathoner mice’s blood, they found 235 different proteins, 23 of which were scarcer and 26 more abundant in marathoner mice than in couch-potato mice. Several of the differently elevated proteins were linked to the complement cascade, which is a collection of roughly 30 blood-borne proteins that interact to kick-start the immune response to infections. Chronic inflammation caused by abnormal complement activation appears to hasten the progression of several neurodegenerative diseases, according to Wyss-Coray.
A blood-borne protein
The anti-inflammatory impact of clusterin, a single protein found in marathoner mice’s plasma, was largely negated when it was removed from sedentary mice’s brains. No other protein examined in the same way got the same result.
Clusterin, a complement cascade inhibitor, was found in much higher concentrations in marathoners’ blood than in couch potatoes’ blood.
Clusterin attaches to receptors found on brain endothelial cells, the cells that line the brain’s blood vessels, according to further research. The majority of Alzheimer’s patients have inflamed blood endothelial cells, according to Wyss-Coray, whose research has revealed that blood endothelial cells may transmit chemical signals from circulating blood into the brain, including inflammatory signals.
Clusterin, when injected outside the brain, was able to diminish brain inflammation in two separate strains of lab mice that had been provoked with either acute bodywide inflammation or Alzheimer’s-related chronic neuroinflammation.
Separately, the researchers discovered that 20 military veterans with moderate cognitive impairment, a precursor to Alzheimer’s disease, had raised clusterin levels in their blood after completing a six-month aerobic exercise program.
According to Wyss-Coray, a drug that boosts or mimics clusterin’s binding to its receptors on brain endothelial cells could help reduce the progression of neuroinflammation-related neurodegenerative illnesses like Alzheimer’s.
Source: Nature
Image Credit: Getty
You were reading: A blood-borne protein provides the same benefits as physical activity