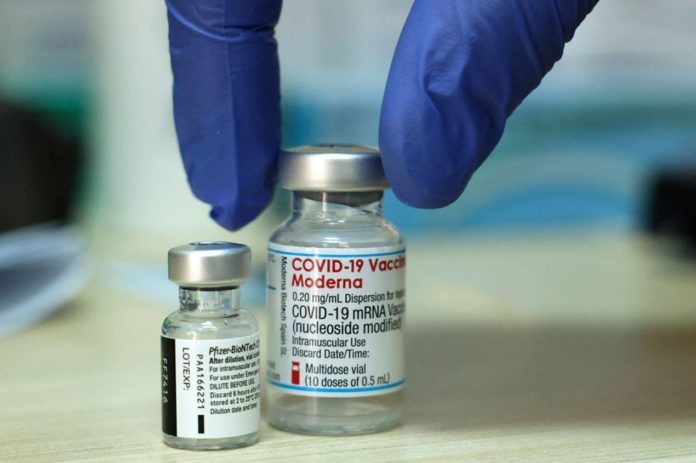
According to Stanford University School of Medicine research, allergic reactions to the new mRNA-based COVID-19 vaccines are rare, normally minor, and manageable, and should not discourage patients from getting vaccinated.
The study, published in JAMA Network Open, looked at 22 probable allergic responses to the first 39,000 doses of Pfizer and Moderna COVID-19 vaccines delivered to Stanford health care practitioners shortly after the vaccines were approved for emergency use by the Food and Drug Administration.
The majority of participants who suffered reactions in the research were allergic to a substance that helps stabilise the COVID-19 shots; they did not have allergies to vaccine components that confer immunity against the SARS-CoV-2 virus. Furthermore, these allergic reactions occurred as a result of an indirect activation of allergy pathways, making them easier to treat than typical allergic reactions.
According to Nadeau, the research also reveals how vaccine manufacturers may reformulate vaccines to make them less likely to cause allergic reactions.
Delivery of protein-making instructions
COVID-19 vaccines based on messenger RNA give protection by encoding molecular instructions for protein production. Because mRNA in vaccines is fragile, it is wrapped in bubbles of lipids (fatty substances) and sugars to keep it stable. When the vaccine is injected into a person’s arm, the mRNA can infiltrate surrounding muscle and immune cells, where it can produce noninfectious proteins similar to those seen on the surface of the SARS-CoV-2 virus. The proteins cause an immunological response, allowing the person’s immune system to recognize and combat the virus.
According to the federal Vaccine Adverse Event Reporting System, the rates of severe vaccine-related anaphylaxis (allergic responses severe enough to cause hospitalization) are 4.7 and 2.5 instances per million doses for the Pfizer and Moderna vaccines, respectively. However, the federal system does not record all adverse reactions to vaccines, and those that are mild or moderate are often missed.
To gain a better understanding of allergic reactions to the new vaccines – how common they are and how severe they are – the researchers examined the medical records of 38,895 health care workers who received doses of mRNA-based COVID-19 vaccines at Stanford Medicine between December 18, 2020, and January 26, 2021. The injections contained 31,635 Pfizer vaccine doses and 7,260 Moderna vaccine doses.
The researchers examined the medical records of vaccine recipients for treatment of allergic responses and determined which reactions were linked to the vaccines. Twenty-two patients, 20 of whom were women, experienced possible allergic responses, which manifested as distinct symptoms within three hours of receiving the doses. The researchers examined the medical records of recipients for the following symptoms: hives; swelling of the mouth, lips, tongue, or throat; shortness of breath, wheezing, or chest tightness; or changes in blood pressure or loss of consciousness. Only 17 of the 22 patients experienced symptoms consistent with an allergic response. Three recipients were given epinephrine, which is generally given for severe anaphylaxis. All 22 people have healed completely.
15 of the 22 patients had physician-documented history of previous adverse reactions, including 10 to antibiotics, 9 to foods, and 8 to nonantibiotic drugs. (Some individuals were allergic to more than one sort of food.)
The researchers conducted additional laboratory tests on 11 people to ascertain what type of allergic reaction they had and what provoked their allergy: Was it one of the bubble’s inert sugar or lipid ingredients, or something else in the vaccine?
Skin-prick tests were performed on trial participants, in which a doctor injected small amounts of possible allergens into their skin, such as lipids, sugars (polyethylene glycol or polysorbates), or the complete vaccination. Skin-prick testing reveals allergic reactions mediated by immunoglobin E, or IgE; these reactions are often linked with the most severe allergies.
On skin-prick tests, none of the recipients reacted to the vaccine’s inert elements, and just one recipient’s skin reacted to the entire COVID-19 vaccine. Following blood tests, the immunisation recipients were found to have insignificant amounts of IgE antibodies against the vaccine components.
Because the skin tests could not explain the mechanism of the recipients’ allergic reactions, the researchers moved on to another form of a diagnostic test. Blood samples from vaccine recipients were collected for testing of allergic activation of immune cells known as basophils. Ten of the eleven individuals’ blood samples revealed a reaction to the inert component polyethylene glycol (PEG), which is used in both the Pfizer and Moderna vaccines. Furthermore, when the full mRNA vaccination was combined with their own basophils, all 11 patients experienced basophil activation.
All 11 subjects showed significant levels of IgG antibodies against PEG in their blood; IgG antibodies help activate basophils under certain conditions, and this discovery indicates that the people were likely susceptible to PEG prior to getting their shots.
“What’s important is what we didn’t find, as much as what we did find,” Nadeau said. “It does not seem that the mRNA itself causes the allergic reactions.”
Furthermore, the findings reveal that reactions to the COVID-19 vaccines were not always the most severe type of allergic reaction, which is excellent news for vaccine safety, she says. Allergic reactions caused by IgG and basophils can be treated with antihistamines, fluids, corticosteroids, and strict monitoring, which means that many people who experienced a reaction to their first vaccine dosage can safely receive a second dose under medical supervision.
PEG is commonly used as a stabilizer in-home items, cosmetics, and pharmaceuticals, and women are more likely to be exposed to significant amounts of the material, which may explain why women experience more vaccination allergies. (Repeated exposure to a drug can occasionally sensitise the immune system and cause allergies.) Because the majority of the reactions were to PEG rather than the vaccine’s active ingredients, vaccine manufacturers can likely reformulate the vaccinations with new stabilisers that are less likely to induce allergies, according to Nadeau.
Image Credit: Getty