A bacterium found in the gut microbiome of mice can boost the immune system’s ability to combat colon cancer cells, say University of Pittsburgh School of Medicine researchers.
The study found that Helicobacter hepaticus increased adaptive immune response and selective activation of Helper T cells and antibody-producing B cells, shrinking colon cancers and extending mouse survival.
The groundbreaking study supports using gut microbiota to treat advanced colon cancer cancers resistant to medication and immunological treatments.
“Altering the gut microbiome doesn’t have to rely on serendipity to get a therapeutic advantage,” says Dr. Timothy Hand, corresponding author.
“Instead of using fecal transplants and hoping to get the right microbial composition, we now are much better positioned to develop effective drugs designed based on molecules produced by beneficial bacteria.”
Colorectal cancer is a common and dangerous disease that resists immunotherapy due to the tumor’s capacity to alter its microenvironment and avoid immune identification. Oncologists must use crude treatments like surgery, chemotherapy, and radiation therapy to aid these patients, all of which have terrible side effects. Making non-responsive tumors sensitive to immune treatments could prove revolutionary.
Some people with colorectal cancer have better treatment outcomes than others, and the gut microbiome could be the key to unlocking the enigma.
Pitt researchers colonized the guts of mice with colon cancer with H. hepaticus, a bacterium that lives in thick mucus in the gut lining and generates a robust immune response, to see if altering the composition of bacterial populations in the colon could improve anti-tumor immunity.
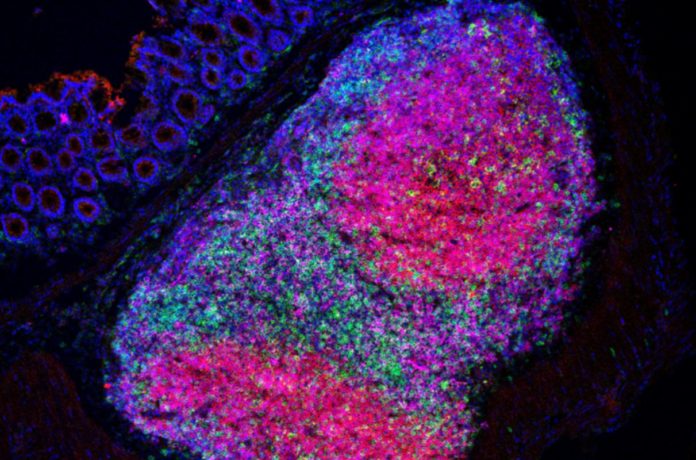
The addition of H. hepaticus lowered the frequency and size of tumors while also extending the lives of the animals. Scientists noticed an increase in the number of Helper T cells, B cells, and natural killer (NK) cells infiltrating the tumor site, as well as the formation of highly organized structures that create a favorable environment for immune cell maturation and indicate that cancer treatments will be more effective.
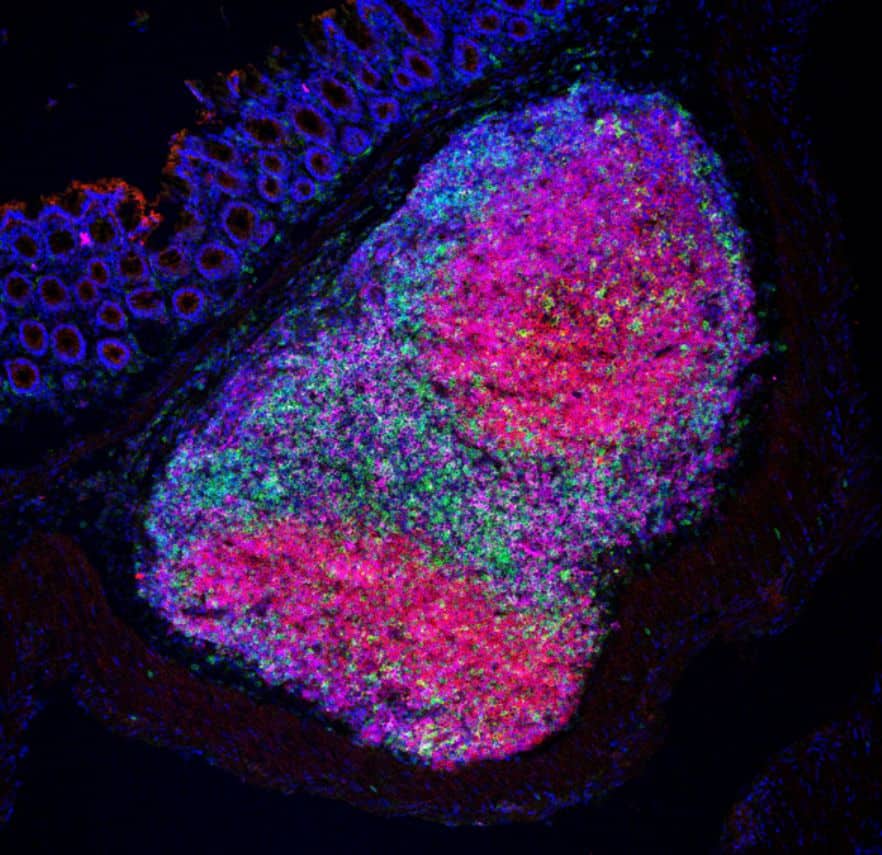
The researchers found no evidence of increased activation of cytotoxic T cells, which are typically targeted by immune treatments, implying that the strategy for colorectal cancer should be changed to prioritize Helper T cells instead.
“Ignoring the influence of gut bacteria on the success of cancer therapies seems like a massive oversight,” says lead author Dr. Abigail Overacre-Delgoffe.
“We need to think about all the things that patients go through day to day that can cause treatments to succeed or fail. We can’t ignore the bacteria anymore—they influence everything.”
Source: 10.1016/j.immuni.2021.11.003
Image Credit: Abigail Overacre-Delgoffe
You were reading: Borrowed bacteria induces strong immune response against cancer cells in the colon