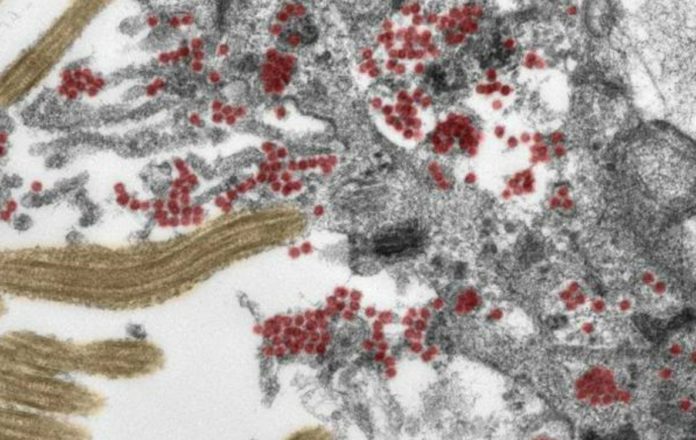
A new study from the Charité University Hospital in Berlin has focused its research on how covid-19 infects the brain and how the immune system responds to the virus and shows that coronavirus is not purely respiratory
There are countless diseases derived from the coronavirus, from lungs and the central or peripheral nervous system to cognitive, muscle and swallowing. It can damage multiple organs and systems of the patient, lung, liver, kidney, heart… More than one in three people with covid-19 report neurological symptoms such as loss or change in sense of smell or taste, headaches, fatigue, dizziness and nausea. In some patients, the disease can even cause a stroke or other serious conditions. Until now, researchers had suspected that these manifestations should be caused by the virus entering and infecting specific brain cells. But how does SARS-CoV-2 get there?
A new study from the Charité University Hospital in Berlin has focused its research on how covid-19 infects the brain and how the immune system responds to the virus. The results, which show that it enters through the nerve cells of the olfactory mucosa, have been published in ‘Nature’ and, for the first time, researchers have been able to produce microscope images of intact coronavirus particles within the olfactory mucosa. Thus they show that the disease caused by the virus is not purely respiratory.
As part of this research, experts from the fields of neuropathology and forensic medicine have analyzed tissue samples from the olfactory mucosa from four different brain regions of 33 patients with an average age of 72 years who had died in Charité or the University Medical Center of Gottingen after contracting the coronavirus.
Using special tissue marking dyes, the researchers analyzed different neuroanatomical structures that connect the eyes, mouth and nose to the brain stem, and the olfactory mucosa was the one that showed the highest viral load. All were found both within nerve cells and in nearby supporting or epithelial cells.
“These data support the idea that SARS-CoV-2 is capable of using the olfactory mucosa as a port of entry to the brain,” explains Dr Frank Heppner, in charge of the study, adding that “this is also supported by the close anatomical proximity “of the mucosal cells, blood vessels and nerve cells in the area.
“Once inside the mucosa, the virus appears to use neuroanatomical connections, such as the olfactory nerve, to reach the brain,” he continues. “It is important to note, however, that the patients with covid-19 involved in this study had suffered the disease seriously, belonging to that small group of patients in whom the disease is fatal. It may not be possible, therefore, transfer the results of our study to cases with mild or moderate disease“.
How the virus moves from nerve cells has not yet been fully clarified, but according to neuropath and study author Helena Radbruch, “It is suggested that the virus moves from one nerve cell to another to reach the brain”. “However, it is likely that the virus is also transported through the blood vessels, as evidence of the virus was also found on the walls of the blood vessels in the brain.”
Researchers also studied how the immune system responds to infection. Thus, in addition to finding evidence of activated immune cells in the brain and olfactory mucosa, they detected immune signals from these cells in the brain fluid.
In some cases, researchers also found damaged tissue caused by a stroke as a result of obstruction of a blood vessel by a blood clot. “In our eyes, the presence of SARS-CoV-2 in the nerve cells of the olfactory mucosa provides a good explanation of the neurological symptoms found in patients, such as loss of sense of smell or taste,” Heppner says.
“We also found SARS-CoV-2 in areas of the brain that control vital functions, such as breathing. It cannot be ruled out that, in patients with severe coronavirus, the presence of the virus in these areas of the brain will have an exacerbated impact on respiratory function, which adds to respiratory problems due to the lung infection itself,” he adds and concludes that this can also explain problems with cardiovascular function.