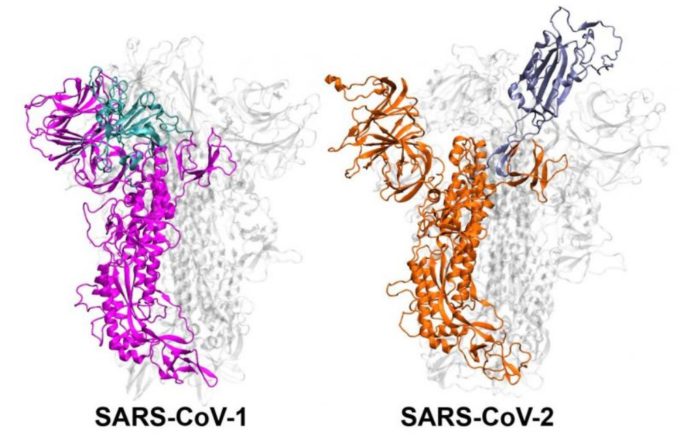
Coronavirus outbreaks have occurred periodically, but none have been as devastating as the COVID-19 pandemic.
Researchers at the University of Arkansas have discovered one of the reasons that probably makes SARS-CoV-2, the virus that causes COVID-19, much more infectious than SARS-CoV-1, which caused the SARS outbreak of 2003.
- Does This Mean We Stopped Being Animal and Started Being Human Due to ‘Copy Paste’ Errors?
- The One Lifestyle Choice That Could Reduce Your Heart Disease Risk By More Than 22%
- Aging: This Is What Happens Inside Your Body Right After Exercise
- Immune-Boosting Drink that Mimics Fasting to Reduce Fat – Scientists ‘Were Surprised’ By New Findings
- Gun Violence in America: What They Don’t Talk About at the Debate
The first step in coronavirus infection is for the virus to enter cells. For this entry, the spike proteins on the outside of the SARS-CoV virus must be repositioned. Scientists know the position of the “inactive” and “active” states of the spike proteins of both the SARS-CoV-1 and SARS-CoV-2 viruses, but these scientists wanted to study how the spikes moved from one position to another and the dynamics of those movements. For this, they resorted to molecular simulations.
“We discovered in these simulations that SARS-CoV-1 and SARS-CoV-2 have completely different ways of changing their shape, and on different time scales. SARS-CoV-1 moves faster, turns on and off, which does not give it that much time to adhere to the human cell because it is not so stable. SARS-CoV-2, on the other hand, is stable and ready to attack,” explains one of the research leaders, Mahmoud Moradi.
There is a region in the tail of the spike protein that has been largely ignored in research, according to Moradi, but that piece is important in the stability of the protein.
Mutations in that region could affect transmissibility and are worth paying attention to. The other implication of his research is that “we could design therapies that alter the dynamics and make the inactive state more stable, thus promoting the deactivation of SARS-CoV-2. That is a strategy that has not yet been adopted,” Moradi explains.
It is valuable to be able to do this type of simulation, according to the scientist, in the event that a new coronavirus emerges, or that SARS-CoV-2 mutates, in order to be able to predict whether the new virus or variant could be greater in terms of transmissibility and infection.
- Does This Mean We Stopped Being Animal and Started Being Human Due to ‘Copy Paste’ Errors?
- The One Lifestyle Choice That Could Reduce Your Heart Disease Risk By More Than 22%
- Aging: This Is What Happens Inside Your Body Right After Exercise
- Immune-Boosting Drink that Mimics Fasting to Reduce Fat – Scientists ‘Were Surprised’ By New Findings
- Gun Violence in America: What They Don’t Talk About at the Debate
Now they have begun to study the new variant ‘B.1.1.7’ of SARS-CoV-2, identified for the first time in the United Kingdom, in the laboratory to detect differences in its movements.