Medical research has altered the course of the outbreak, and experimental technologies that have accelerated the development of vaccines have hooked rocket boosters to scientific aspirations. Is it possible that we are about to experience a golden era of new vaccines?
If you go to the leading edge of vaccine development, you will see Prof Dame Sarah Gilbert of the Jenner Institute, who was key in shaping the Oxford vaccine.
In only 65 days, the Oxford team had a vaccine ready to begin clinical trials thanks to a new approach. More than 1.5 billion jabs have been delivered globally in collaboration with pharma giant AstraZeneca.
How they did it?
Oxford’s coronavirus vaccine was developed using a totally new method known as “plug-and-play.”
The new generation of vaccines are highly adaptable and quick to manufacture. “It’s like decorating a cake,” said Prof Gilbert.
The traditional technique of developing vaccines requires going back to the basic ingredients and starting from scratch with each vaccination. It’s just like mixing a bench of flour, sugar, eggs, and butter. The next stage is to either kill or weaken the culprit virus or other disease-causing microorganisms in order to create a vaccine.
Consider the two seasonal flu vaccines administered each year. Adult vaccines are produced by culturing influenza viruses within eggs. Purified and dead viruses are then used to create the vaccine.
Although the nasal spray for children contains live viruses, they have been rendered weak and unstable so that they may develop in the lower temperatures of the nose but not in the warmer temperatures of the lungs.
However, starting from scratch with each new illness is very time consuming and there are many potential pitfalls.
With this new approach, most of the work has already been done – the cake has already been baked, and it just has to be “decorated” to fit its goal.
“We’ve got the cake and we can put a cherry on top, or we can put some pistachios on top if we want a different vaccine, we just add the last bit and then we’re ready to go,” Prof Gilbert told Inside Health.
The “cake” – or platform, to use the technical term – of the Oxford vaccine is a virus that causes the common cold in chimps. It has been genetically engineered to be safe and incapable of infecting humans. The “decoration” refers to whatever genetic blueprint is required to educate the immune system to attack. A blueprint like this is put to the cake, and the work is done.
Two other important Covid vaccines, one produced by Pfizer-BioNTech and the other by Moderna, use a different kind of highly adaptable plug-and-play vaccine technology. All of these technologies should make developing future vaccines faster and simpler.
What’s next?
“There’s a lot of vaccine development that we need to do now that we can do it,” said Prof Gilbert.
The official “priority pathogens” are at the top of her list of targets. While Covid was a surprise, these are the known dangers that have the potential to trigger major outbreaks and possibly pandemics in the future.
Including Mers, Lassa, Crimean-Congo hemorrhagic fever, Nipah, Zika, Ebola, Rift Valley Fever, Chikungunya, Dengue, Hantavirus, Plague, Marburg, Q Fever
Some of this work has already begun. Using its plug-and-play technology, Oxford has begun clinical trials for a plague vaccine. The plague was notorious for causing the Black Death outbreak, which killed hundreds of millions of people. Separately, Moderna is considering developing a Nipah vaccine using its own mRNA technology. The virus kills up to three-quarters of those who get infected.
However, the biggest obstacle to fighting these illnesses will remain the same as it has always been – funding. They strike some of the poorest areas of the globe, and there is fear that research will not be sponsored even if a pandemic occurs.
And, although vaccines technology has advanced, the old foes haven’t changed, and some have cunning peculiarities that make them impossible to defeat.
All vaccines need a target, known as an antigen, to educate the immune system to attack.
Despite all of the difficulties Covid has created, the virus was a very basic beast with a clear target antigen. The virus’s outer surface is coated with spike proteins. So all researchers had to do was plug in the spike protein’s genetic blueprints, educate the body to recognize it, and be quite sure that the vaccine would function.
However, with some more complicated microbes, such as the three major killers, malaria, HIV, and TB, the target antigen is not apparent. HIV is an ever-changing target. It is a shape-shifter that quickly mutates to change its appearance and deceive our immune system. It’s difficult to put a finger on it.
We already have malaria and TB vaccines, but they are far from perfect.
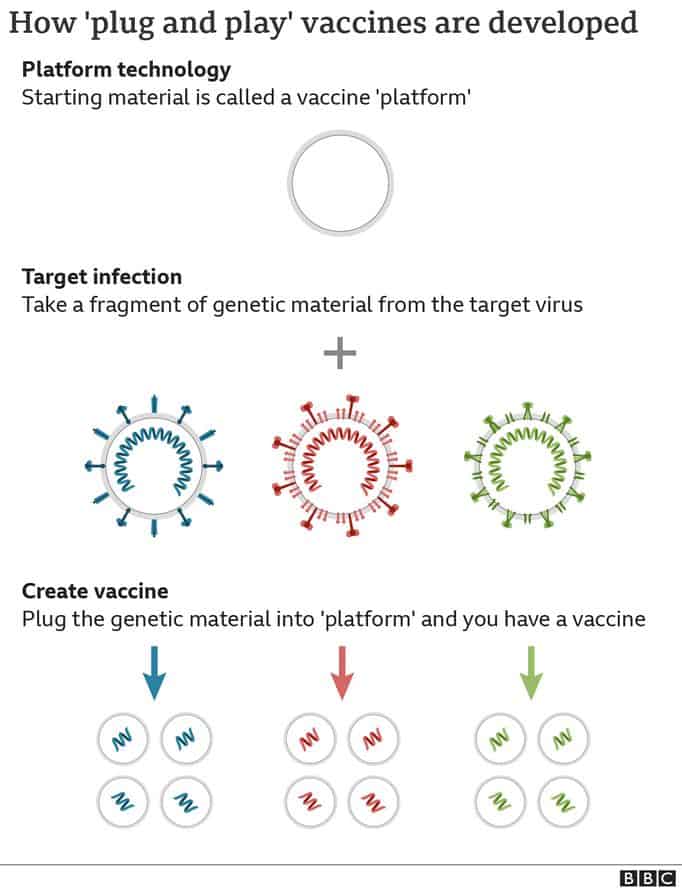
Image credit: Getty
You were reading: Covid vaccines may help fight against viruses and other disease-causing microbes
