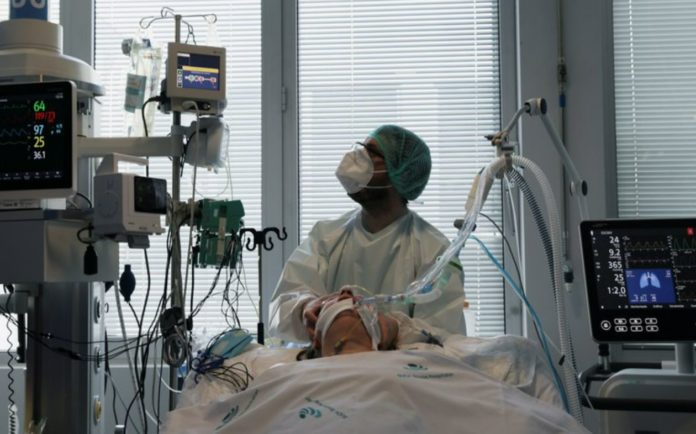
Stronger signaling proteins, increased T-cell activation, and increased susceptibility to autoimmunity are just some of the ways that women’s bodies seem to respond differently than men’s
Among the many health disparities that characterize the COVID-19 pandemic, one that has received special attention is the difference in outcomes between men and women. As of February last year, researchers noted that although men and women contracted COVID-19 at similar rates, men seemed much more likely to die from the disease.
- Does This Mean We Stopped Being Animal and Started Being Human Due to ‘Copy Paste’ Errors?
- The One Lifestyle Choice That Could Reduce Your Heart Disease Risk By More Than 22%
- Aging: This Is What Happens Inside Your Body Right After Exercise
- Immune-Boosting Drink that Mimics Fasting to Reduce Fat – Scientists ‘Were Surprised’ By New Findings
- Gun Violence in America: What They Don’t Talk About at the Debate
Evidence of the gap has continued to emerge as COVID-19 data sets have expanded, warns research published in the scientific journal The Scientist. For example, data aggregated by the Sex, Gender, and COVID-19 Project indicates that, although statistics vary substantially between countries in the world, men with the disease are about 20 percent more likely to be hospitalized than women. Once hospitalized, men are more likely to require intensive care and, once there, are more likely to die.
One person who was not surprised by these differences is Sabra Klein, a biologist at Johns Hopkins Bloomberg School of Public Health. Klein has been studying immune responses to viral infections for more than two decades and says COVID-19 is helping to highlight an important truth in the biology of infectious diseases: that viruses and other pathogens do not affect women and men alike. And at least part of that difference cannot be explained simply by differences in exposure or risk-related behavior between women and men; it all comes down to biology.
Once a controversial idea, the concept of gender differences in immune function has taken hold in the research community in recent years. Retrospective analyzes of data from the 2003 SARS and the 2013-2014 MERS coronavirus outbreaks, for example, have revealed that, among detected cases, men had a higher risk of death than women. And several other viruses, such as hepatitis C, are known to cause more serious infections in men. On the other hand, autoimmune diseases such as lupus, multiple sclerosis, and rheumatoid arthritis, which in many cases are believed to arise from the overactivation of antiviral immune pathways, are much more common in women, leading Klein and other researchers to theorize that scientists could be looking at two sides of the same coin.
With the pandemic helping to draw attention to the influence of sex on disease outcome, Klein and others have been investigating the mechanisms underlying the differences in immune responses between XY men and XX women. In both humans and other mammals, her findings reveal fundamental distinctions at the genetic, cellular, and organism levels that, according to the specialist, could influence the way scientists approach the study, treatment, and prevention of human infectious diseases. “SARS-CoV-2 just changed the discussion enormously. My hope is that in the future, after the pandemic, this will start to spread and we will start to see these considerations more broadly in immunology and infectious diseases.”
Documenting gender differences in immune responses
Perhaps the most consistent result researchers have found when studying functional variation in the mammalian immune system is that females tend to elicit “stronger” immune responses to viral infections than males, warns Marcus Altfeld, an immunologist at the Heinrich-Pette-Institut in Hamburg.
This difference is particularly evident in the cells involved in the innate immune system, which tend to respond more quickly in women to the stimulation of viruses that bind to the receptors of those cells and, once stimulated, launch a greater production of molecules antiviral signaling. “This is really the first step in the immune response against a virus,” Altfeld explains.
His group has focused on the toll-like receptor 7 (TLR7), a protein involved in the detection and response to single-stranded RNA in cell cytoplasm, an early warning sign that a virus has invaded the cell. As early as 2009, Altfeld, then at Harvard Medical School, and his colleagues observed that certain TLR7-bearing immune cells known as plasmacytoid dendritic cells from women produced significantly more interferons in response to stimulation with HIV RNA fragments than men’s cells.
- Does This Mean We Stopped Being Animal and Started Being Human Due to ‘Copy Paste’ Errors?
- The One Lifestyle Choice That Could Reduce Your Heart Disease Risk By More Than 22%
- Aging: This Is What Happens Inside Your Body Right After Exercise
- Immune-Boosting Drink that Mimics Fasting to Reduce Fat – Scientists ‘Were Surprised’ By New Findings
- Gun Violence in America: What They Don’t Talk About at the Debate
Other researchers have found that neutrophils, the most abundant type of white blood cell in the mammalian immune system, appear to respond better to interferon signaling if samples are taken from women. Specifically, female cells show stronger upregulation of multiple genes involved in immune defense, according to a study published last year by Mariana Kaplan and her colleagues at the National Institute of Arthritis and Musculoskeletal and Skin Diseases.
Research in recent years has also pointed to gender differences in the development of adaptive immunity. Klein, who uses flu vaccines to experimentally study the responses of mice to immune stimulation, has found that females tend to generate higher neutralizing antibody responses. The T cells normally associated with immune responses adaptive but can also play a role in innate immunity, also show specific features of sex. For example, multiple studies point to a higher number of helper T cells, that promote the activation of large bands of the adaptive immune system, in girls and adult women than in men.
Klein says that the stronger immune responses illustrated by these and similar studies are likely a double-edged sword from a health perspective. On the one hand, the increased immune activation of women could help limit the amount of virus in the body, an effect seen in people with HIV, for example, since women tend to have much lower viral loads than men in the first years of infection. In addition, females appear to generate better protective antibody responses than males after vaccination against influenza, yellow fever, dengue, and several other viruses. On the other hand, the same biology likely predisposes women to diseases stemming from overactive immune responses as well, Klein notes.
“The downside to this strong immunity is that 80 percent of all patients with autoimmune diseases are women,” she stresses.
“We are much more likely to have autoimmune diseases; we are much more likely to have multiple autoimmune diseases.”
Women are also at higher risk of disease progression in some infections caused by interactions of the immune system, such as HIV infection, which progresses to AIDS faster in women than in men. Altfeld’s group has reported clinical data showing that women with HIV have greater T-cell activation, a key factor in predicting disease progression, than men with the same viral load, and concluded in their study of 2009 that stronger TLR7 signaling in women probably explained part of this difference.
Although many details of SARS-CoV-2 infection have not yet been described, several studies have already hinted that discrepancies in immune system function may be responsible for some of the gender differences in COVID-disease outcome, including the fact that men appear to be at higher risk of death. Akiko Iwasaki of Yale University and her colleagues recently showed that hospitalized patients with COVID-19 had higher numbers of activated T cells than male patients, for example, reinforcing the idea that women generate a stronger immune response to SARS-CoV-2 and may be better protected from serious illnesses, says Iwasaki to The Scientist.
- Does This Mean We Stopped Being Animal and Started Being Human Due to ‘Copy Paste’ Errors?
- The One Lifestyle Choice That Could Reduce Your Heart Disease Risk By More Than 22%
- Aging: This Is What Happens Inside Your Body Right After Exercise
- Immune-Boosting Drink that Mimics Fasting to Reduce Fat – Scientists ‘Were Surprised’ By New Findings
- Gun Violence in America: What They Don’t Talk About at the Debate
Meanwhile, early studies of protracted COVID-19, a loosely defined condition involving symptoms that last for weeks to months after infection, already indicate a female bias. Although the condition is far from understood, some researchers have speculated that the disease could be mediated by T cells and could involve an attack on autoantigens (molecular markers on a person’s own cells) just like an autoimmune condition.