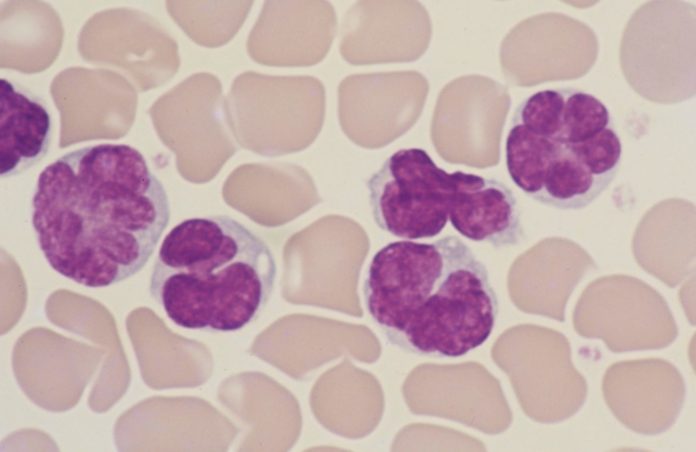
A multinational team of researchers has identified how the HTLV-1 virus produces rare leukemia in some people, providing insights on how to prevent it from happening in the future.
The researchers, led by Imperial College London and Kumamoto University in Japan, employed single-cell analysis to demonstrate how the virus over activates T-cells, which are crucial immune cells in our blood, causing them to become malignant.
Adult T-cell leukaemia/lymphoma (ATL) occurs in approximately 5% of people infected with the HTLV-1 virus, but only after several decades of infection. HTLV-1 preferentially infects T-cells and changes them into leukemia cells, but the time lag makes determining how this transformation occurs extremely challenging.
ATL can progress slowly or rapidly, but there is no conventional treatment for high-grade ATL, and the infection recurs frequently following treatment with chemotherapy and antiviral medicines.
The findings, published today in The Journal of Clinical Investigation, show that the virus hijacks the activation machinery of T-cells, enabling them to remain activated at high levels and eventually become cancerous.
“While only a small percentage of people with HTLV-1 viral infections go on to develop adult T-cell leukaemia/lymphoma, there are estimated to be around five to ten million carriers of the virus worldwide, and in some areas it is endemic – for example there are around one million cases in Japan,” said Co-lead researcher Professor Yorifumi Satou.
“There is therefore a great need to understand how the virus turns our T-cells against us in the progression to cancer. Our work highlights a key mechanism for this change and provides us with new directions to search for ways to interfere with the process, potentially preventing the cancer from developing,” added another co-lead researcher Dr Masahiro Ono, from the Department of Life Sciences at Imperial.
Leukaemias are malignancies that arise from blood or bone marrow cells and are distinguished by a significant increase in the number of aberrant white blood cells. T-cells are specialized white blood cells that help the body fight off intruders such as viruses and bacteria.
The HTLV-1 virus attaches itself to a specific type of T-cell and initially remains in a ‘latent’ state, not releasing any new virus particles or causing any harm. For many of these virus carriers, this never changes, but in about 5% of carriers, the virus reawakens after decades of dormancy and disrupts T-cell function.
The researchers examined almost 87,000 T-cells from virus-free donors, healthy viral carriers, and ATL patients. They read the RNA (a smaller type of DNA) from these cells to determine how the virus and T-cells interacted.
They discovered that in individuals who developed ATL, HTLV-1 activated and over-reacted infected T-cells, enabling them to over-produce proteins that keep them proliferating and allowing them to evade other sections of the immune system that would normally remove rogue cells.
The researchers believe that these modifications made the hyperactive T-cells more sensitive to DNA damage, such as that caused by chemical agents or radiation, accelerating their progression to cancer.
According to the authors, more research into the processes involved will provide the groundwork for potential new treatment options.
Dr Ono further added: “For example, the chronic activation of T-cells could be halted by molecules that block signalling pathways that tell the cells to activate. Alternatively, treatments could target the proteins the activated T-cells create to help them proliferate.”
Source: 10.1172/JCI150472
Image Credit: Dr Uchiyama
You were reading: How a virus turns our immune cells into cancer revealed by researchers