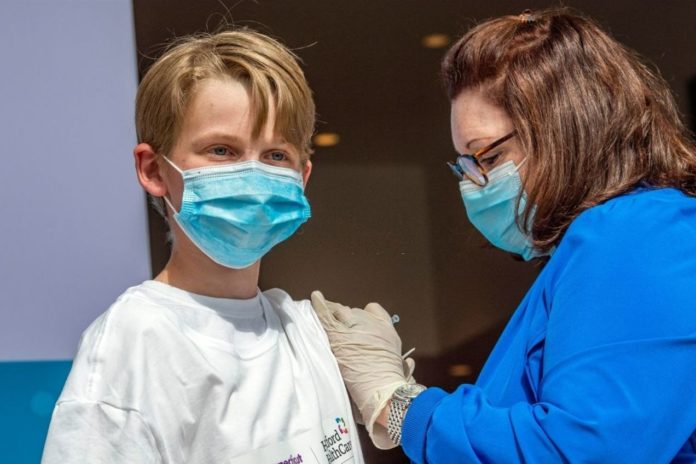
Most people who receive the COVID-19 vaccine are well aware of the usual side effects following the first and second Pfizer and Moderna doses: shoulder pain, possibly a headache, muscular pain or exhaustion.
However, a much rarer reaction has recently sparked concern: myocarditis, or inflammation of the heart muscle.
Here’s everything you need to know about myocarditis and its connection to COVID-19 and vaccinations.
Myocarditis
It may be the first time you’ve heard of it, but myocarditis is not a novel disease. It can be caused by a variety of factors, including viral infections, some medicines, some autoimmune illnesses, and exposure to environmental pollutants such as heavy metals and radiation. According to the National Heart, Lung, and Blood Institute, myocarditis can also be caused by a vaccination reaction, albeit this is uncommon.
The Centers for Disease Control and Prevention (CDC) is “actively monitoring” reports of myocarditis and pericarditis (inflammation of the sac that surrounds the heart) in a small group of people who received mRNA vaccines from Pfizer and Modern; in most cases, the disease develops after the second injection. According to the EPA, 12.6 instances of myocarditis occur for every 1 million doses of COVID-19 mRNA vaccination administered to people aged 12 to 39.
A more recent study published in JAMA Internal Medicine discovered a rate of 5.8 myocarditis cases per million in adults from the second dose.
“The other thing that’s notable is that the vast majority of cases are self-resolving,” according to Dr. Nisha Gilotra, an associate professor at Johns Hopkins Medicine, which means that most patients improve rapidly after rest and without any major medical treatment.
“In fact, [myocarditis] is probably underreported because so many of the cases can be asymptomatic or subclinical. A very rare proportion will [have symptoms that bring them into a health care setting] or be on the more severe spectrum,” Gilotra further adds.
Vaccine vs. myocarditis
According to Dr. Manesh Patel, chief of cardiology at Duke University School of Medicine, elderly people are reasonably concerned about anything linked to the heart, given that heart disease is the leading cause of death and that adults 65 and over are more likely to suffer from it. However, when it comes to vaccine-related myocarditis, the elderly are mainly unaffected.
The vast majority of vaccine-related cases have been reported in teenagers and young adults. According to a CDC report released in June, the rate of myocarditis from the second dose of COVID-19 mRNA vaccines given to men ages 12 to 29, and 2.4 per million from the second dose given to men 30 years of age or older, was 40.6 cases per million; the rates for women in these age groups were 4.2 and 1 per million for the second dose, respectively.
People aged 12 to 17 have been shown to have the highest rates. There were approximately 63 occurrences of myocarditis per million doses of the COVID-19 mRNA vaccine delivered in this group.
These data reflect what the National Heart, Lung and Blood According to the National Heart, Lung, and Blood Institute, the following is true for the majority of instances of myocarditis: It is more common in young adults. And the explanation is most likely related to the immunological response. According to the CDC, inflammation is caused by the body’s immune system in both myocarditis and pericarditis, which is triggered by infection or another source. Furthermore, younger people have more strong immunological responses than their peers.
“That’s why younger people seem to be more resistant to getting as sick with COVID than older people who don’t have this robust immune system,” says Patel.
“It’s also maybe why you have younger people having a little bit more myocarditis than older people.”
COVID vs. myocarditis
Despite this, major health experts, doctors, pharmacists, and nurse associations across the country urge that individuals aged 12 and up get vaccinated, citing that the benefits outweigh the minor risk. (Vaccines are still being investigated in children under the age of 12.)
One reason is that COVID-19 is more likely to produce myocarditis than the vaccination, and the damage to the heart caused by the infection may be more severe.
“Really, when we see severe myocarditis, or this severe inflammatory response in the heart, we’re seeing it with actual acute COVID infection,” says Gilotra.
Another reason: COVID-19 can cause a variety of serious complications aside from myocarditis, such as brain and lung damage, particularly in older adults and people with underlying conditions such as heart disease, so people with existing heart problems should not be discouraged from getting vaccinated.
“I’ve been advising my patients broadly — those with heart disease and even those without who are older — to get the COVID vaccine. I am not concerned about myocarditis,” says Patel.
Even younger people, who are less likely to become seriously ill from a coronavirus infection, are at risk for COVID-19, which includes multisystem inflammatory syndrome, or MIS-C, a disease that is “far more severe than the mostly self-resolving cases of vaccine-related myocarditis,” according to Gilotra. There is also the issue of long-term COVID, which refers to the disease’s chronic symptoms that millions of COVID survivors have described following a coronavirus infection.
According to research, vaccines avoided roughly 5,700 occurrences of COVID-19, as well as 215 hospitalizations and two fatalities, among teenagers who suffered the highest rate of myocarditis after vaccination (about 63 cases per million doses of the second dose delivered). Furthermore, those who developed myocarditis after vaccination have not experienced any long-term effects that we’ve been able to measure at this point,” according to Dr. Yvonne Maldonado, an infectious disease expert and professor of Pediatrics, Epidemiology, and Population Health at Stanford Medicine.
Other Potential causes of Myocarditis or Heart Inflammation
The cause of myocarditis is often unknown. There are numerous probable causes, but the likelihood of getting myocarditis is extremely low, according to Mayo Clinic.
Myocarditis can be triggered by a mixture of reasons, including:
- Viruses. Many viruses are commonly associated with myocarditis, including the viruses that cause the common cold (adenovirus); COVID-19; hepatitis B and C; parvovirus, which causes a mild rash, usually in children (fifth disease); and herpes simplex virus.Gastrointestinal infections (echoviruses), mononucleosis (Epstein-Barr virus) and German measles (rubella) also can cause myocarditis. It’s also common in people with HIV, the virus that causes AIDS.
- Bacteria. Bacteria that can cause myocarditis include staphylococcus, streptococcus, the bacterium that causes diphtheria and the tick-borne bacterium responsible for Lyme disease.
- Parasites. Among these are such parasites as Trypanosoma cruzi and toxoplasma, including some that are transmitted by insects and can cause a condition called Chagas disease. Chagas disease is much more common in Central and South America than in the United States, but it can occur in travelers and in immigrants from that part of the world.
- Fungi. Yeast infections, such as candida; molds, such as aspergillus; and other fungi, such as histoplasma, often found in bird droppings, can sometimes cause myocarditis, particularly in people with weakened immune systems.
Myocarditis also sometimes occurs if you’re exposed to:
- Medications or illegal drugs that might cause an allergic or toxic reaction. These include drugs used to treat cancer; antibiotics, such as penicillin and sulfonamide drugs; some anti-seizure medications; and some illegal substances, such as cocaine.
- Chemicals or radiation. Exposure to certain chemicals, such as carbon monoxide, and radiation can sometimes cause myocarditis.
- Other diseases. These include disorders such as lupus, Wegener’s granulomatosis, giant cell arteritis and Takayasu’s arteritis.
So it’s not just COVID vaccines, there are many risk factors involved in the development of heart inflammation.
“The benefits really outweigh the risks related to vaccination,” Gilotra says.
“And the reassuring thing is that so much of the 65-plus population has been vaccinated, so we have a lot of compelling data in this age group about the safety and the impact of vaccination in the pandemic.”
And If you still have any concerns, consult with a trusted healthcare physician.
“They can talk to you about your individual risk and any concerns and hesitancies you might have,” Gilotra says.
Image Credit: Getty
You were reading: Risk of developing inflammation of the heart muscle after COVID-19 vaccine, virus and other potential causes