Treatment for pancreatic cancer is quite challenging. By the time it is discovered, cancer has usually progressed to an advanced stage, and patients seldom survive more than a year following diagnosis.
The first-line treatment is a strong chemotherapy regimen, but the side effects can be severe, and many cancers do not respond to treatment.
Now, scientists at Washington University School of Medicine in St. Louis have discovered a drug combination that renders pancreatic cancer cells more vunerable to chemotherapy.
As a result of their research on mice, scientists found evidence that this drug combo may also help to decrease some of the harmful side effects of the regularly used pancreatic cancer chemotherapy cocktail FOLFIRINOX (a mixture of folinic acid 5-fluorouracil irinotecan and oxaliplatin).
The research was published in the journal Science Translational Medicine on December 1.
“There is a tremendous need for new and better therapies for pancreatic cancer,” says senior author and medical oncologist Kian-Huat Lim, MD, PhD, an associate professor of medicine.
“The drugs that we use now are powerful but often cause severe side effects, making it impossible to add more chemotherapy. This new drug appears to weaken the cancer cells and make them more sensitive to this particular chemotherapy regimen. In fact, the mice treated with chemotherapy plus this drug appear to be healthier than mice receiving chemotherapy alone, so there’s a chance the new drug is mitigating side effects.”
The medicine, ATI-450, is an anti-inflammatory treatment that is also being tested in clinical studies as a rheumatoid arthritis treatment.
FOLFIRINOX is the first-line treatment for pancreatic cancer, but only around one out of every three patients will see their tumor shrink. Even so, the response is only good for six to seven months. Nausea, vomiting, diarrhea, exhaustion, hair loss, low blood counts, and poor appetite are all frequent side effects.
In their study, the authors found that a chemical called MK2 is important for pancreatic tumor cells to survive chemotherapy as part of their research. The molecule is highly activated in pancreatic cancer cells, where it activates survival-promoting signaling pathways and inhibits cell death.
Since ATI-450 is an MK2 inhibitor, it is a promising candidate for testing against these cancer cells.
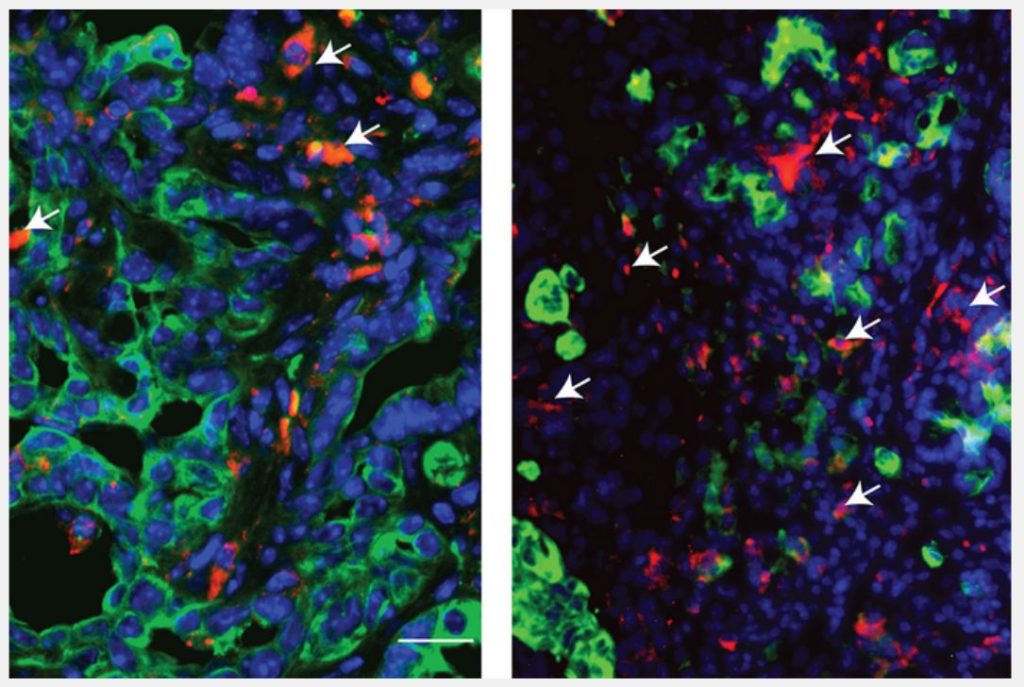
“MK2 turns on pro-survival mechanisms that allow cancer cells to adapt to the severe stresses of chemotherapy,” says first author and medical oncologist Patrick M. Grierson, MD, PhD, an assistant professor of medicine.
“It also inhibits a type of cell death called apoptosis, thereby preventing tumor cells from dying in the face of chemo. This new drug inhibits MK2, so when the mice receive the drug at the same time that they receive chemotherapy, the tumor cells are much more susceptible to dying.”
Lim and Grierson, both treat pancreatic cancer patients at the Siteman Cancer Center at Barnes-Jewish Hospital and Washington University School of Medicine, and their colleagues evaluated the drug’s effects in pancreatic cancer cell lines grown in the laboratory, mice harboring human pancreatic cancer cells, and mice that developed pancreatic cancer naturally due to a genetic predisposition to the disease.
In comparison to chemotherapy alone, the combination of ATI-450 and chemotherapy resulted in a nearly 50% reduction in tumor size. Additionally, mice receiving the combo treatment lived longer, on average 41 days after treatment began, compared to 28 days for mice receiving chemotherapy alone.
“A nearly 50% increase in survival is a significant improvement,” says Grierson.
“On top of that, it’s impressive that the drug did not worsen side effects. There is a concern with chemotherapy for pancreatic cancer that incorporation of additional drugs will make the treatment even less tolerable. We monitored blood counts and assessed toxicities on the small intestine and colon where we often see limiting toxicities, and the adverse effects were no worse with the combination treatment.”
Lim further adds: “A lot of the side effects of chemotherapy are due to inflammation caused by molecules called cytokines. A benchmark for success in treating rheumatoid arthritis, which this drug was originally developed for, is the reduction of those cytokines. It’s possible we’re seeing the same effect in these mice.”
The researchers plan to continue exploring ATI-450 for pancreatic cancer, particularly if this medicine in combination with other investigational treatments, such as immunotherapies, can be effective. Additionally, the researchers stated that the medicine may improve treatment for other tumors that are treated with comparable chemotherapy regimens, such as colon and other gastrointestinal malignancies.
Image Credit: Getty
You were reading: This new drug combo makes pancreatic cancer cells more chemosensitive