It is no secret that heart disease is a top killer of the elderly, and that, owing to changes in modern lifestyles, it is also on the rise among the young.
Heart disease is notoriously difficult to diagnose since its symptoms come and go so suddenly. This has increased interest in long-term cardiac imaging and other sophisticated, inclusive, non-invasive, and cost-effective monitoring devices like this wearable gadget.
Cardiac imaging is one of the best ways to find and treat problems with the heart before they get worse.
“The heart undergoes all kinds of different pathologies,” points out co-author Hongjie Hu.
According to the author, cardiac imaging will show what’s really going on. Whether the volume changes are caused by a strong but normal contraction of heart chambers or by an emergency cardiac morphological problem, real-time image monitoring of the heart gives a clear picture of the whole situation.
Cardiac imaging is an important clinical tool that is used to check the long-term health of the heart, find problems as they happen, and help people who are very sick.
This new wearable heart monitor offers real-time, automated analysis of the heart’s pumping activity, even during physical activity, without the need for invasive procedures.

The wearable heart monitoring device employs ultrasound to continually record pictures of the four chambers of the heart from various angles and analyzes a clinically relevant subset of the images in real time using a custom-built artificial intelligence technology. The project builds on what the team has already done to make imaging technology for deep tissues that can be worn.
“The increasing risk of heart diseases calls for more advanced and inclusive monitoring procedures,” says lead author Sheng Xu, adding, “by providing patients and doctors with more thorough details, continuous and real-time cardiac image monitoring is poised to fundamentally optimize and reshape the paradigm of cardiac diagnoses.”
Existing non-invasive methods, on the other hand, have limited sampling capabilities and only give limited information. The wearable device created by Xu’s team makes it possible to do safe, non-invasive, and high-quality cardiac imaging, producing pictures with a high level of contrast, spatial resolution, and temporal resolution.
“It also minimizes patient discomfort and overcomes some limitations of noninvasive technologies such as CT and PET, which could expose patients to radiation,” adds co-autho Hao Huang.
The sensor’s one-of-a-kind design makes it particularly well-suited for use with moving bodies. According to Xiaoxiang Gao, a postdoctoral researcher in the Xu group at UC San Diego, the device may be mounted to the chest with little restriction to the participants’ mobility, even giving a continuous recording of cardiac events before, during, and after exercise.”
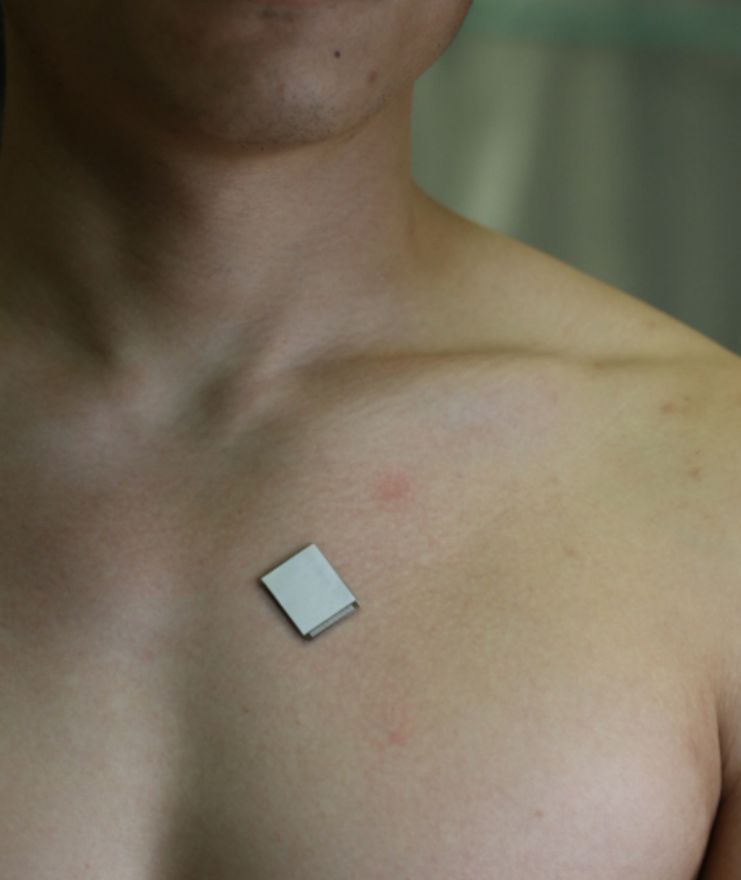
The new system gets information from a patch that is as soft as human skin and is made to stick well. The patch is about the size of a postage stamp, measuring 1.9 cm (L) × 2.2 cm (W) x 0.09 cm (T). It transmits and receives the ultrasonic waves that are utilized to produce a continuous stream of real-time pictures of the heart’s anatomy. This ultrasonic patch sticks nicely to human skin even while being stretched out and is soft and flexible.
Using ultrasound, the system can look at the left ventricle of the heart from two different angles. This makes it possible to get more clinically useful images than before. As an example of a use case, the team showed how imaging the heart while it is working out is not possible with the rigid, heavy equipment used in clinical settings.
Three things determine how well the heart works: stroke volume, ejection fraction, and cardiac output (the volume of blood the heart pumps out every minute). Stroke volume is the amount of blood the heart pumps out with each beat. Ejection fraction is the percentage of blood pumped out of the left ventricle of the heart with each beat.
The team led by Xu has created an algorithm to enable autonomous, real-time processing with the help of AI.

According to Mohan Li, a master’s candidate in the Xu group at UC San Diego, “a deep learning model automatically segments the shape of the left ventricle from the continuous image recording, extracting its volume frame-by-frame and yielding waveforms to measure stroke volume, cardiac output, and ejection fraction.”
According to Ruixiang Qi, a master’s candidate in the Xu group at UC San Diego, the AI component specifically incorporates a deep learning model for picture segmentation, an algorithm for heart volume computation, and a data imputation technique.
“We use this machine learning model to calculate the heart volume based on the shape and area of the left ventricle segmentation.”
It is the first time that a deep learning model for image segmentation has been implemented in a portable ultrasound system. It makes it possible for the device to give accurate and continuous waveforms of key cardiac indices in different physical states, such as when the person is standing still or after exercise. This has never been done before.
So, this technology can make curves of these three indices continuously and without making any changes to the data. This is possible because the AI part processes the constant stream of images to make numbers and curves.
In order to make the platform, the team had to deal with some technical problems that required them to make careful decisions. The researchers employed a piezoelectric 1-3 composite bonded with Ag-epoxy backing as the material for transducers in the ultrasonic imager to create the wearable device itself, lowering risk and enhancing effectiveness compared to earlier techniques. Wide-beam compounding transmission gave them the best results when deciding how to set up the transducer array for transmission. For machine-learning-based picture segmentation, they chose FCN-32 out of nine well-known models since it had the greatest accuracy.
The patch is now wired to a computer, allowing the machine to automatically download data while the patch is still active. A wireless circuit for the patch has been created by the team and will be featured in a future publication.
Xu and engineer Shu Xiang created Softsonics, a UC San Diego spinoff, to commercialize this technology.
The work was described in the Jan. 25 issue of the journal Nature.
Source: 10.1038/s41586-022-05498-z
Image Credit: David Baillot/ UC San Diego Jacobs School of Engineering
