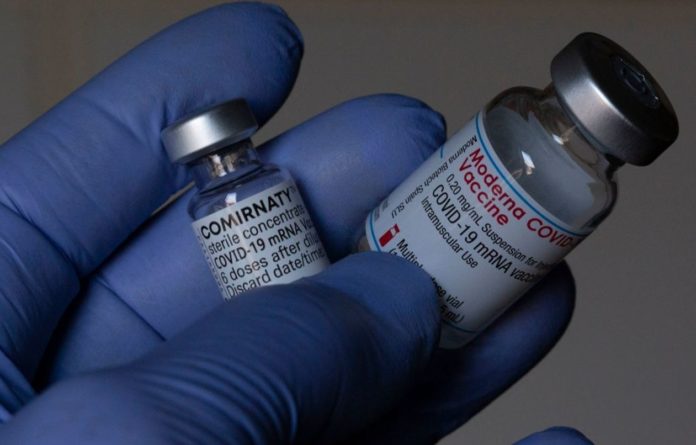
The first direct comparison of Pfizer and Moderna vaccines
Researchers evaluated the electronic health records of veterans who had received each vaccine in the first head-to-head comparison of the efficiency of the Pfizer-BioNTech and Moderna COVID-19 vaccines. Both vaccines were highly efficient at protecting COVID-19-related complications such as infection, hospitalization, and death.
The Moderna vaccine, on the other hand, was found to provide an increased level of protection, including a 21% reduction in the risk of documented infection and a 41% reduction in the risk of hospitalization, according to the research team, whose findings were published in the New England Journal of Medicine on December 1, 2021.
“Both vaccines are incredibly effective, with only rare breakthrough cases,” says Dr. J.P. Casas, a member of the research team comprised of experts from the United States Department of Veterans Affairs (VA), Harvard T.H. Chan School of Public Health, and Brigham and Women’s Hospital.
However, “regardless of the predominant strain—Alpha earlier and then Delta later—Moderna was shown to be slightly more effective,” says Casas, an epidemiologist and associate professor at Brigham and Women’s Hospital and Harvard Medical School, as well as the executive director of the VA’s Million Veteran Program for genetics and health research.
The researchers conducted their comparative effectiveness analysis to see which of the two mRNA vaccines is more successful. The effectiveness of the intervention was evaluated using five COVID-related outcomes: documented COVID-19 infection, symptomatic disease, hospitalization, intensive care unit admission, and mortality. The research used electronic health information from United States veterans who got one of the two COVID-19 vaccines between early January and mid-May 2021.
As actually planned, the research concentrated on the dominant Alpha form at the time. The study compared 219,842 Pfizer vaccine recipients to the same number of Moderna vaccine recipients. The two groups were matched on a variety of clinical and demographic variables known to influence outcome.
The estimated risk of recorded infection throughout the 24-week follow-up period was 4.52 incidents per 1,000 persons in the Moderna vaccination group and 5.75 events per 1,000 people in the Pfizer vaccine group. This equates to an excess of 1.23 documented incidences of illness per 1,000 individuals in the Pfizer group. Additionally, the authors reported an increase in symptomatic COVID-19 (0.44 events), hospitalization (0.55 events), intensive care unit admission (0.10 events), and mortality (0.02 events) per 1,000 persons in the Pfizer group compared to the Moderna group, but these differences were minor.
This pattern of a decreased risk for Moderna was confirmed in a subsequent round of research over a time period during which Delta was the predominant strain. In this comparison, the Pfizer vaccine had an increased risk of recorded infection of 6.54 occurrences per 1,000 persons over 12 weeks, compared to Moderna. Given the limited time window available for this supplemental investigation, the researchers focused exclusively on infection. Additionally, the estimations were deemed less exact due to the reduced sample size for this investigation.
Prior randomized trials comparing the mRNA vaccines to placebo demonstrated that both were highly successful against symptomatic COVID-19 infection (95 percent efficacy for Pfizer-BioNTech, 94 percent for Moderna), and similar benefits were reported in real-world vaccine use.
“Given the high effectiveness of both the Moderna and Pfizer vaccines, confirmed by our study, either one is recommended to any individual offered a choice between the two,” says the study’s first author, Dr. Barbra A. Dickerman.
“However, while the estimated differences in effectiveness were small on an absolute scale, they may be meaningful when considering the large population scale at which these vaccines are deployed. This information may be helpful for larger decision-making bodies.”
The large VA records system, which contains millions of patients countrywide, enabled the collection of an extremely large sample size. This enabled the investigation to detect even minute differences in the efficacy of the Pfizer and Moderna vaccinations. The researchers employed a technique called causal inference to replicate as nearly as feasible a randomized trial—the gold standard in health research. Causal inference is a subset of data analysis that enables researchers to make confident inferences about cause and effect.
A significant hurdle for this study was ensuring that the vaccine groups were equivalent in terms of non-vaccine-related characteristics that may predict infection or disease severity. The VA databases enabled the researchers to properly characterize and closely match recipients of each vaccine type in terms of age, sex, race, geographic region, and other characteristics associated with COVID-19-related outcomes.
“After this careful matching, we found that the two vaccine groups were extremely similar in terms of variables with respect to an extensive set of demographic, geographic, and health-related attributes,” says Dickerman.
“This allowed our observational analysis to produce exceptionally credible results during a global emergency, when answers are needed fast and randomized trials can be impractical.”
As the global pandemic unfolds, the research team is examining the comparative safety and efficacy of the Pfizer and Moderna vaccines. Comparative safety, according to Dickerman, is an “additional piece of the puzzle to support vaccine decision-making.”
The study authors concluded, “Given the high effectiveness and safety profile of both mRNA vaccines, either one is strongly recommended.”
Source: New England Journal of Medicine
Image Credit: Getty
You were reading: Which COVID-19 vaccine is more effective? study reveals