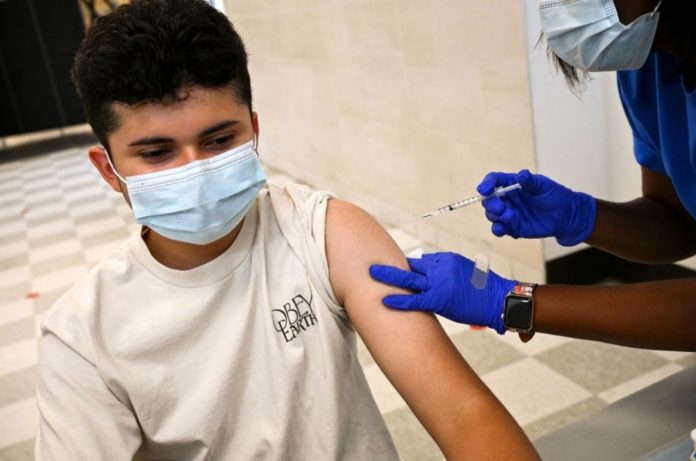
According to a review of research, those who develop more than five symptoms of Covid-19 in the first week are more likely to experience long COVID, regardless of age or gender.
Patients with long-COVID have symptoms that sometimes last for months.
The study, published in the Journal of the Royal Society of Medicine (JRSM), summarised current data on the prevalence, consequences, and treatment of long COVID.
- Does This Mean We Stopped Being Animal and Started Being Human Due to ‘Copy Paste’ Errors?
- The One Lifestyle Choice That Could Reduce Your Heart Disease Risk By More Than 22%
- Aging: This Is What Happens Inside Your Body Right After Exercise
- Immune-Boosting Drink that Mimics Fasting to Reduce Fat – Scientists ‘Were Surprised’ By New Findings
- Gun Violence in America: What They Don’t Talk About at the Debate
The researchers from the University of Birmingham in the United Kingdom highlighted that the review’s pooled prevalence data shows the 10 most common symptoms of long-COVID.
These are fatigue, shortness of breath, muscle pain, cough, headache, joint pain, chest pain, altered smell, diarrhoea and altered taste, said the researchers.
The team found two types of long COVID symptom clusters: those that include only of tiredness, headache, and upper respiratory problems, and those that include multi-system complaints such as persistent fever and gastroenterological symptoms.
There is evidence that the impact of acute COVID-19 on patients, regardless of severity, extends beyond hospitalisation in the most severe cases, to ongoing impaired quality of life, mental health and employment issues
explained Olalekan Lee Aiyegbusi of the University of Birmingham is the study’s main author.
People living with long COVID generally feel abandoned and dismissed by healthcare providers and receive limited or conflicting advice.
More than one-third of participants in one of the trials included in the analysis reported feeling unwell or in poorer clinical condition eight weeks after the onset of COVID-19.
The researchers observed that neither the molecular or immunological processes behind long COVID, nor the reason for why some individuals are more vulnerable to these effects, are known at the moment, posing a barrier to the development of treatments.
“It is essential we act quickly to address these issues,” said Shamil Haroon, the study’s co-principal investigator from the University of Birmingham..
In contrast to other coronaviruses, the researchers indicate that individuals with long COVID may also have a disease trajectory comparable to that of patients with SARS or MERS in the long term.
People living with long COVID generally feel abandoned and dismissed by healthcare providers and receive limited or conflicting advice
Aiyegbusi said.
They cite research indicating that about 25% of individuals hospitalised with SARS or MERS had decreased lung function and exercise ability six months after discharge.
The wide range of potential symptoms and complications patients with long COVID may experience highlights the need for a deeper understanding of the clinical course of the condition
said Melanie Calvert, a professor at the University of Birmingham and co-principal investigator of the research.
There is an urgent need for better, more integrated care models to support and manage patients with long COVID to improve clinical outcomes
Calvert added.