Mitochondria are the organelles in human cells that make energy. They used to be free-living organisms that moved into early eukaryotic cells more than a billion years ago. Since then, they have become one with their hosts, which is a classic example of symbiotic evolution. They now depend on proteins made in the nucleus of their host cell to work properly.
Mitochondrial outer membrane proteins are particularly important, as they allow mitochondria to connect with the rest of the cell and participate in immunological functions and apoptosis, a sort of programmed cell death. Over time, cells have developed a specific way to put these proteins, which are made in the cytoplasm of the cell, into the mitochondrial membrane. But it has been a mystery for a long time what that mechanism was and which cells were involved.
Answers to these questions are presented in a recent study from the research groups of Whitehead Institute member Jonathan Weissman and California Institute of Technology professor Rebecca Voorhees. The research, which was published today in the journal Science, demonstrates that a protein known as mitochondrial carrier homolog 2, or MTCH2, which has been associated with numerous cellular functions and even illnesses like cancer and Alzheimer’s, is in charge of acting as a “door” for a variety of proteins to access the mitochondrial membrane.
According to Weissman, who is also a professor of biology at the Massachusetts Institute of Technology and an Investigator of the Howard Hughes Medical Institute, “until now, no one knew what MTCH2 was really doing; they just knew that when you lose it, all these different things happen to the cell.”
It was kind of hard to figure out why this one protein affects so many different things. This study, according to the authors, gives a molecular explanation for why MTCH2 was linked to Alzheimer’s, lipid biosynthesis, and mitochondrial fission and fusion: it was responsible for putting all these different types of proteins in the membrane.
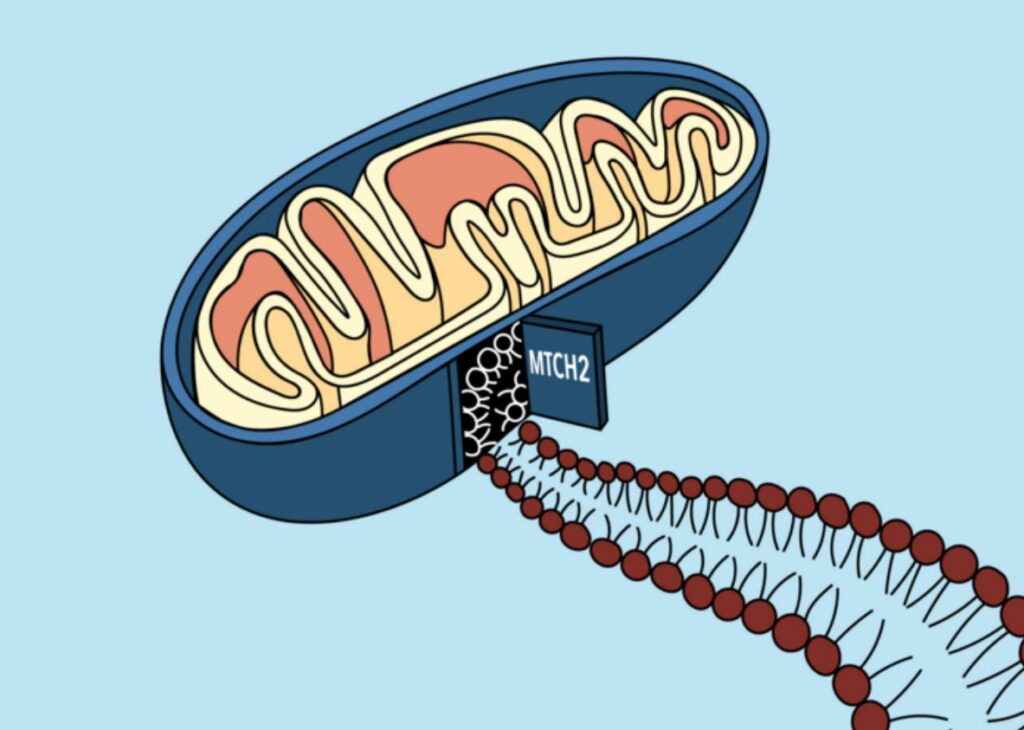
Doorhunting
Alina Guna, a postdoctoral researcher in the Whitehead Lab and the study’s first author, along with Taylor Stevens, a graduate student in the Voorhees Lab, and postdoctoral researcher Alison Inglis chose to use a method known as the CRISPR interference (or CRISPRi) screening approach, developed by Weissman and collaborators, to investigate how proteins from the cytoplasm, specifically a class known as tail-anchored proteins, were being inserted
Guna explained, “The CRISPR screen lets us systematically get rid of every gene, and then look and see what happened [to one specific tail-anchored protein].
“We found one gene, MTCH2, where when we got rid of it there was a huge decrease in how much of our protein got to the mitochondrial membrane. So we thought, maybe this is the doorway to get in.”
To prove that MTCH2 was a doorway into the mitochondrial membrane, the researchers did more tests to see what happened when MTCH2 wasn’t in the cell. They discovered that for tail-anchored membrane proteins to translocate from the cytoplasm to the mitochondrial membrane, MTCH2 was both required and sufficient.
It is most likely because of its unique structure that MTCH2 is able to transport proteins from the cytoplasm into the mitochondrial membrane. Alpha Fold, an AI system that predicts a protein’s structure from its amino acid sequence, was used to analyze the protein’s sequence, and the results showed that it is hydrophobic, making it ideal for insertion into the oily membrane, but it does have a single hydrophilic groove that could be used by other proteins.
“It’s basically like a funnel,” Guna added. “Proteins come from the cytosol, they slip into that hydrophilic groove and then move from the protein into the membrane.”
Guna and her colleagues came up with another experiment to prove that this groove was important to how the protein worked.
“We wanted to play around with the structure to see if we could change its behavior, and we were able to do that,” Guna highlighted. “We went in and made a single point mutation, and that point mutation was enough to really change how the protein behaved and how it interacted with substrates. And then we went on and found mutations that made it less active and mutations that made it super active.”
The new study is useful for more than just answering a basic question about mitochondria.
“There’s a whole lot of things that come out of this,” Guna remarked.
One way that MTCH2 could be used to combat cancer is by inserting proteins that are essential for apoptosis, a sort of programmed cell death. By giving leukemia cells a mutation that alters the function of MTCH2, Guna explained, “we can make them more sensitive to a cancer treatment.” The mutation causes MTCH2 to act more “greedy” and insert more substances into the membrane; some of these substances that have inserts are similar to pro-apoptotic factors, so that cells are thus more likely to die; this is excellent in the context of a cancer treatment.
The work also makes people wonder how the function of MTCH2 changed over time. The solute carrier protein family, which transports various chemicals across cellular membranes, is where MTCH2 originated.
“We’re really interested in this evolution question of, how do you evolve a new function from an old, ubiquitous class of proteins?” Weissman said.
Furthermore, there is still much to learn about how mitochondria communicate with other parts of the cell, including how they respond to stress and cellular changes as well as how proteins initially end up in mitochondria.
Weissman thinks “that [this paper] is just the first step. This only applies to one class of membrane proteins — and it doesn’t tell you all of the steps that happen after the proteins are made in the cytoplasm. For example, how are they ferried to mitochondria? So stay tuned — I think we’ll be learning that we now have a very nice system for opening up this fundamental piece of cell biology.”
Image Credit: Getty
You were reading: ‘Until Now, No One Knew’ This One Protein Affects All Strange Things That Happen To The Cell