A team of Swedish scientists have found out how human skin can withstand staphylococcus aureus. It turned out that cells of the lower layers of the skin produce a pro-inflammatory cytokine that attracts immune cells. This explains why a deadly super-microbe can occasionally settle on people’s skin without harming their health.
According to WHO, Methicillin-resistant staphylococcus aureus (MRSA) is one of the ten most dangerous microbes for humanity. It is responsible for three-quarters of inflammation of the skin and soft tissues, and infection with them often leads to the death of patients. It is all the more surprising that approximately every fifth person has Staphylococcus aureus among the permanent inhabitants of the nasal cavity. And judging by the presence of antibodies to it in the blood, almost every one of us sooner or later came across this microbe.
Apparently, a person has some kind of mechanism to combat a dangerous bacterium. Anette Schulz of the Karolinska Institute and her colleagues suggested that human skin can serve as protection against staphylococcus aureus. To test how bacterial colonization of the skin occurs, the researchers transplanted areas of healthy human skin into immunodeficient mice, and after that, they placed Staphylococcus aureus on it.
Scientists found that during the first five days after the resettlement, the bacterium successfully multiplies on the surface of the skin, but by the tenth day, it almost completely disappears. At no point in time did staphylococcus penetrate into the inner layers of the skin; each time it was found only on the surface of the outer stratum corneum. This effect was reproduced for different skin donors, which means that the matter is not in the immunity of a particular person, but in some kind of universal mechanism.
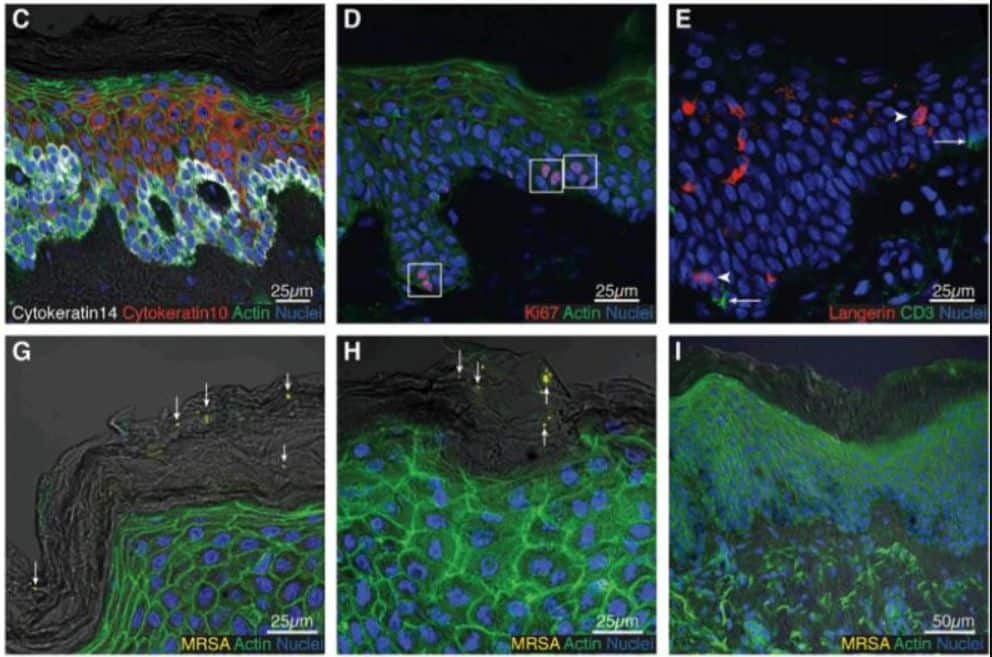
The researchers homogenized areas of the skin that resisted staphylococcus and found an increased concentration of interleukin-8 in it. This is a pro-inflammatory cytokine that is designed to attract immune cells to the site of infection, primarily neutrophils. When scientists stained skin preparations with characteristic markers, they really saw neutrophils – both in the dermis and in the epidermis of the skin itself.
Interleukin-8 is a human cytokine, mice have only its analogue, but its concentrations remained practically unchanged even when the skin was populated with staphylococcus. The number of other murine cytokines also remained constant. Therefore, the researchers concluded that the main “alarm” comes from human cells, that is, from skin cells. When scientists blocked interleukin-8 with antibodies or caused neutropenia in mice – a deficiency of neutrophils – they stopped resisting infection, and the number of bacteria on the skin surface did not decrease over time.
Thus, scientists have discovered in human skin a new mechanism of protection against staphylococcus, which is not found in mice, but acts only if there is a sufficient number of immune cells on alert. Nevertheless, scientists behind this research note that some strains of Staphylococcus aureus produce substances that are toxic to human neutrophils, so the real picture of the battle of immunity with a super microbe can be even more complicated.