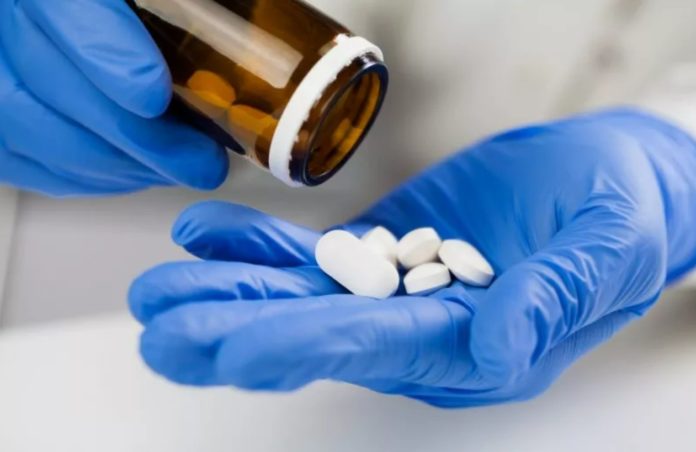
The Food and Drug Administration (FDA) approved the antiviral pill molnupiravir, made by Merck and Ridgeback Biotherapeutics, for emergency use in the United States on December 23, 2021, after an advisory panel narrowly recommended the treatment.
The pill is intended for individuals who have mild-to-moderate COVID-19 symptoms and are at a high risk of developing severe disease.
Molnupiravir is only accessible by prescription and should be started as soon as feasible following a COVID-19 diagnosis and no later than five days after the onset of symptoms. The FDA made it clear when it approved the medicine that it will only be used by high-risk persons for whom alternative therapies aren’t “accessible or clinically appropriate.” It should not be used for longer than five days in a row.
For Molnupiravir also known as LAGEVRIO, there are only a few clinical studies available. Serious and unexpected side effects that have not been previously recorded with the usage of LAGEVRIO may develop.
The usage of LAGEVRIO is not advised during pregnancy. LAGEVRIO may harm a fetus if given to a pregnant woman, according to evidence from animal reproduction research. There is no human data on the use of LAGEVRIO in pregnant women to assess the risk of serious birth abnormalities, miscarriage, or other negative maternal or fetal outcomes.
According to Jay Grobler, associate vice president, infectious diseases and vaccines, Merck Research Laboratories, “Phase 3 study in patients with mild to moderate COVID-19, LAGEVRIO, an investigational oral antiviral medicine, cleared infectious SARS-CoV-2 faster than placebo among patients who had infectious virus at baseline, resulting in no infectious virus detected at Day 3, 5 or 10.”
He added: “These data reinforce our confidence in the potential of LAGEVRIO as a part of the solution to the COVID-19 pandemic.”
Although the findings are encouraging, some scientists are concerned that using the drug could promote the formation of new COVID-19 variants and subvariants, such as Omicron and its mutations, that are highly transmissible and/or bypass vaccine protection to some extent.
Molnupiravir works by preventing the SARSCoV2 virus, which causes COVID-19, from replicating once it has entered the body’s cells. It accomplishes this by causing mistakes in the virus’s genetic code. When enough faults are introduced, the virus is unable to replicate, and the patient is able to rid their body of the pathogen.
However, some researchers have warned that new variants may emerge throughout the mutation process, however other specialists have disregarded such concerns.
Professor Michael Lin of Stanford University says: “I am very concerned about the potential consequences now that molnupiravir has been approved.”
He added: “It would only be a matter of time, perhaps a very short time, before a lucky set of mutations occurs to create a variant that is more transmissible or immunoevasive.”
“Mutations are what naturally create variants of concern that are more contagious or immunoevasive, like Delta or Omicron,” he added. “The drug simply speeds up that natural process. The hope is that over enough days all the viral copies will have so many mutations that none of the copies can function.”
Lin, on the other hand, expressed concern that in the real world, a modified virus could spread from a patient using molnupiravir to another person.
When a patient does not follow the drug’s dosing schedule perfectly, according to Lin, the dangers are increased.
“This treatment is an oral one, so it is going to rely on the patients taking their pills. Patients are notoriously poor at completing a course of pills correctly. They’ll forget, or they’ll feel side effects and stop, or they’ll feel better and think they don’t need to finish the pills.”
“In any of those situations viruses will have picked up some mutations but not enough to kill all the virus copies,” he told Newsweek.
“The survivors are now mutated, perhaps have picked up immunoevasion, and can go on to infect others.
“Even if the drug were great we wouldn’t take such a risk, but this drug is worse than any other drug that’s sought approval for COVID19. It’s completely not worth it.”
Other experts have expressed concern about molnupiravir and its ability to accelerate the formation of new strains, including Dr. William Haseltine, an expert in the COVID-19 pandemic and former professor at Harvard Medical School who is known for his landmark work on HIV/AIDS and cancer.
With molnupiravir, Haseltine claims that patients sweat live virus for two or three days after starting treatment.
“Of all the antiviral drugs I have ever seen, this is by far the most potentially dangerous. The more people that take it, the more more dangerous it will be,” Haseltine added.
Other coronaviruses—the family to which SARS-CoV-2 belongs—could become resistant to molnupiravir, according to research undertaken prior to the pandemic. The drug’s development began in the mid-2010s, with the goal of making it a treatment for influenza.
When the antiviral was tested against two different coronaviruses, MERS-CoV and the mouse hepatitis virus (MHV), researchers discovered a rise in changes, particularly in the crucial spike protein, which allows infections to bind to and enter living cells.
In fact, researchers discovered more than 100 changes in the genome of MERS, which is closely related to SARS-CoV-2. This is more mutations than the Omicron COVID-19 type, which contains a lot of them.
Despite the fact that these experiments revealed a replication disadvantage, the MERS and MHV viruses were nevertheless able to live and multiply.
“While it’s possible that at the optimal concentration, the drug may very well cause enough mutations to prevent replication and onward transmission of [SARS-CoV-2,] the impact of suboptimal doses is still very much unknown,” Haseltine wrote in an article for Forbes.
Officials from the FDA examined Merck’s molnupiravir clinical trial findings for the treatment of SARS-CoV-2 and discovered that virus mutations were more common among those who received the medicine vs those who received a placebo.
Some of these structural alterations were identical to those identified in important COVID-19 variants, such as Delta, according to FDA researchers who told the advisory group at the time of EUA, which voted 13 to 10 in support of proposing emergency authorization. The chance of new variants appearing in individual patients, according to FDA researchers, is negligible.
James Hildreth, president of Meharry Medical College in Tennessee, was one of the panel members who voted nay, saying Merck could do more to estimate the risk of such an incident.
“Even if the probability is very low, one in 10,000 or 100,000, that this drug would induce an escape mutant which the vaccines we have do not cover, that would be catastrophic for the whole world,” he told the panel.
In a statement, a Merck spokesperson said: “There is no evidence to indicate that any antiviral agent has contributed to the emergence of circulating variants. Over the course of the pandemic, variants have emerged due to uncontrolled viral replication and continued transmission caused by an absence of widely available treatment options and low levels of vaccination. Antivirals such as molnupiravir, because they help to address these issues, can form an important part of the solution.”
Several other scientists indicated they were unconcerned about molnupiravir’s ability to produce new, potentially harmful variants.
Dr. Douglas Richman, a professor of pathology and medicine at the University of California San Diego, told Newsweek: “I am personally not concerned that molnupiravir presents a risk for the emergence of resistant viruses of concern.”
The “real concerns,” according to the researcher, are the possible possibility of the medicine damaging human genes and its “less than optimal efficacy.”
The chance of drug-resistant viral changes, according to Dr. John Williams, a pediatrics professor at the University of Pittsburgh School of Medicine, is “low.”
“I and the scientists I am in contact with are not particularly concerned that this drug will fuel the emergence of a new variant of concern. In testing of the drug against SARS-CoV-2 in cells and animals, as well as against other RNA viruses, the drug causes lethal mutations in the viruses and there was a high barrier to developing resistance.”
Even if drug-resistant mutations do emerge, Williams says there’s no reason to believe they’ll act any differently from existing variants.
“In fact, drug-resistant viruses are often ‘weaker’ than the ‘wild type’ viruses,” he added.
For a variety of reasons, Sankar Swaminathan, an infectious disease specialist at the University of Utah School of Medicine, said the appearance of novel variations in molnupiravir patients was “not likely to happen,” at least on a broad scale.
“The high rate at which mutations are induced in the viral genome are likely to lead to so-called catastrophic mutation, which renders the virus incapable of replicating. It is therefore generally unlikely to generate viable viruses capable of surviving and being transmitted at a higher rate than normally occurs during normal untreated infection.”
“We have no evidence that such [new variants] survived treatment in the normal individuals in the study. But the frequency at which these may exist is not known for certain.”
Nonetheless, Swaminathan noted that the chance of developing new variants may be increased in immunocompromised people using the pill, even though the risks are still low.
“Under circumstances where viral elimination is impaired, as we have seen in patients with compromised immune systems, viruses persist and come through each round of antiviral therapy or antibody treatment, having escaped elimination, and with mutations that have been selected to be resistant,” he added. “We simply do not know if this is likely or how often it may happen in the immunocompromised patient.”
Image Credit: Getty
You were reading: As Paxlovid fails, experts question another COVID-19 Anti-Viral Pill: “It’s completely not worth it”