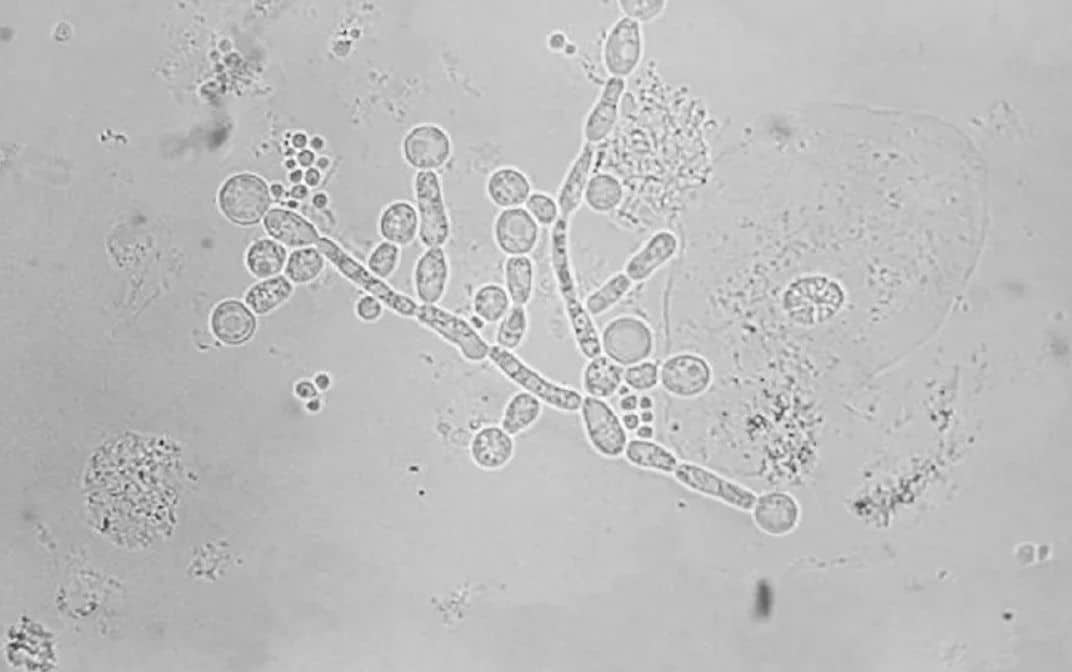
In the midst of a pandemic, a fungal infection is causing major complications in hospitals in Brazil, Italy, Spain and Denmark. Doctors are trying to control it to avoid worsening the situation of critical patients who are hospitalized, including those suffering from COVID-19. Why is this mushroom so powerful?
It seems that the classic fungi that are in the biota of our intestines are now becoming more and more resistant to treatments. When the body functions well, these fungi do not cause any problems, but when there is some imbalance due to chronic diseases or hospitalization for various interventions for a long period of time – as in the cases of COVID-19 – they can enter the streaming blood and cause serious, life-threatening infections.
That’s what’s happening in many hospitals, according to a study published in Frontiers in Cell and Infection Microbiology. The research found that the fungi have the exact same DNA sequence, which could be an indication of the presence of more virulent varieties.
What fungus complicates the COVID-19 pandemic?
They are fungi of the genus Candida, candidemia, as Candida infection in the bloodstream is called, occurs mainly in patients in intensive care units (ICU), as well as in patients undergoing organ transplants and treatments of some types of cancer, such as leukaemia.
How are Candida infections caused?
Most Candida infections occur when the fungus crosses the intestinal barrier and enters the bloodstream due to complications of serious illness and prolonged hospital stay.
However, a part of these infections is due to the so-called breakdown of hygiene techniques by the hands of health professionals, as well as inadequate care while managing patients subjected to invasive medical procedures.
“These factors allow horizontal transmission of these agents to occur between different patients, which explains the presence of groups of infection that affect individuals admitted to the same ward or, less frequently, in different institutions,” said Arnaldo Lopes Colombo from Fundação de Amparo a Pesquisa-São Paulo (FAPESP), a Professor Universidade Federal de São Paulo, São Paulo, Brazil and the only Brazilian co-author of the study.
How is Candida related to COVID-19?
Currently there are a large number of critical patients with COVID-19 hospitalized, which represents “a complication to which the health system must be alert,” said Lopes Colombo.
“These patients require two to three weeks of hospitalization in intensive care units, exposed to antibiotics, immunomodulatory drugs, invasive medical procedures and hemodialysis,” he explained.
How did they identify the fungus?
The researchers analyzed 884 samples from 16 hospitals, in which they identified 723 genotypes of three species: Candida albicans (534 samples), C. parapsilosis (282) and C. tropicalis (68).
In the future, the researchers will conduct a complete genome analysis of a portion of the samples to confirm genetic similarity within groups and refine the microsatellite marker methodology for Candida genetic studies, according to FAPESP. In addition, they will study what makes the clusters so virulent to develop more effective treatments.
“We are observing that the strains involved in cumulus events have a greater capacity to produce biofilm, an extracellular matrix that serves to adhere to surfaces and protect themselves from the inhospitable environment, in this case, the human immune system,” said Colombo.