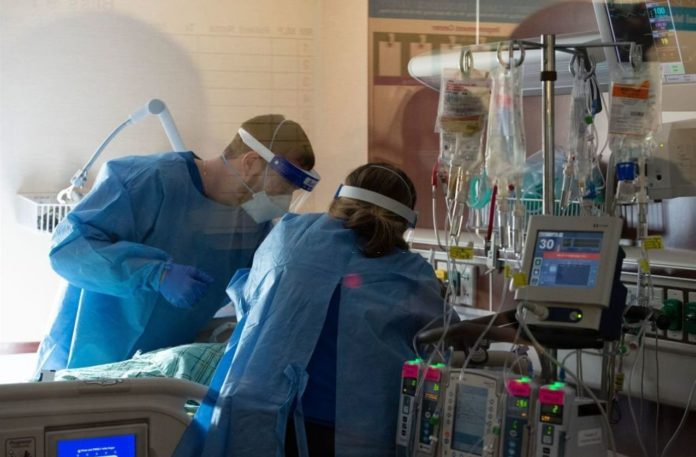
Researchers from the University of Chicago in Illinois and the Providence Research Network in Washington, which is part of one of America’s largest healthcare companies, Providence, discovered that those who had never received any COVID-19 jabs but developed COVID-19 and evolved natural immunity had a longer window of defense against another SARS-CoV-2 infection than those who had mRNA shots-induced immunity.
To date, the probability of reinfection with SARS-CoV-2 among individuals who had never received a COVID-19 vaccination with prior COVID-19 is debatable.
The researchers conducted a survival analysis in a large US population to determine the degree and duration of protection provided by natural immunity in people who had never received any COVID-10 vaccines.
Between October 1, 2020, and November 21, 2021, data from patients tested for SARS-CoV-2 at 1300 locations of care in six western US states in the Providence health care system were used in this novel cohort study.
Patients who had never received a COVID-19 vaccine and showed symptoms that were compatible with COVID-19 at the time of testing were included in this study. Patients were evaluated for subsequent COVID-19 infection for 90 days following their initial SARS-CoV-2 nucleic acid amplification test (NAAT), as defined by a positive SARS-CoV-2 NAAT result in the presence of symptoms.
The researchers compared patients with past COVID-19 (positive for SARS-CoV-2 on their initial test [cases]) to patients who tested negative for SARS-CoV-2 on their initial test (controls) using Cox proportional hazards regression, adjusted for age, sex, race, and ethnicity (based on medical record documentation).
Participants were excluded when they received a COVID-19 vaccine, died, or tested positive for SARS-CoV-2 at their last primary care or inpatient visit during the course of the study (encounters in which clinicians consistently verified jab status using electronic medical records and outside data), or when they received a COVID-19 vaccine, died, or tested positive for SARS-CoV-2.
The level of protection associated with previous COVID-19 was determined as 1 minus the hazard ratio (HR) for COVID-19 among cases vs controls by the research team. The team also calculated a 50-day rolling mean of the protection level and assessed 95 percent CIs with 1000 bootstrap sampling to track protection over time.
The study’s design was approved by the Providence institutional review board, which waived the necessity for informed consent because the trial was deemed low-risk. The study team utilized R, version 4.1.2 (R Foundation for Statistical Computing) for statistical analysis and followed the (STROBE) reporting guidelines.
The researchers found 24 043 cases and 97 572 controls, with 2762 controls (2.8%) developing COVID-19 compared to 98 cases (0.4 percent ). The data reveal that both cases and controls are disease-free.
In the survival model, the HR was 0.15 (95 percent CI, 0.13-0.18) for developing COVID-19, 0.12 (95 percent CI, 0.08-0.18) for hospitalization for COVID-19, and 0.17 for COVID-19 without requiring hospitalization (95 percent CI, 0.13-0.21).
Importantly, prior COVID-19 was linked to an 85 percent reduction in the risk of recurring COVID-19, an 88 percent reduction in the risk of COVID-19 hospitalization, and an 83 percent reduction in the risk of COVID-19 not requiring hospitalization, according to the data. Up to 9 months after initial infection, protection remained steady throughout the research period, with no attenuation.
People who had never received any COVID-19 jabs and had prior symptomatic COVID-19 had an 85 percent lower risk of acquiring COVID-19 than those who had never received any COVID-19 jabs and also had no prior COVID-19, according to the study, which included 121 615 patients with more than 10 million days of follow-up.
Interestingly, previous research into SARS-CoV-2 reinfection protection reported comparable results, with protection associated with natural immunity ranging from 80.5 percent to 100 percent.
Natural immunity was linked to similar protection against mild and severe disease, according to the findings.
mRNA jabs were also found to provide similar long-term protection against severe COVID-19 as found in the study, though jab-associated protection against moderate COVID-19 has been shown to decline after 6 months.
Possible COVID-19 testing or vaccinations at outside health care facilities are study limitations, although undiagnosed infection should have been balanced between cases and controls. Patients who have recovered from COVID-19 may act differently from those who have not, thus causing results to be skewed. The study’s strengths include a large sample size, a lengthy period of follow-up, and the inclusion of only people with symptomatic COVID-19 who had never received any COVID-19 vaccines. This study’s findings could have significant ramifications for vaccine policy and public health.
It’s worth noting that the study was conducted before the highly transmissible omicron variant was discovered in the United States.
“We found that, before the emergence of the omicron variant, natural immunity provided a similar degree of protection against COVID-19 infection as mRNA jabs,” Dr Ari Robicsek, M.D., Providence’s chief medical analytics officer, said. However, “jabs are considerably safer way to acquire that immunity.”
The study, led by a team of expert clinicians and scientists from the Providence Research Network, involved a detailed examination of data from over 100,000 patients tested for SARS-COV-2 at 1,300 sites of care throughout Providence’s extensive health care system between October 1, 2020, and November 1, 2021.
Prior COVID-19 infection was found to be 85 percent protective against reinfection and 88 percent protective against hospitalization, with protection from reinfection lasting up to nine months after the initial infection, as far back as the researchers could look.
This recent study, which is one of the largest of its kind, demonstrates the value of providing researchers with large-scale health-care data, as well as the impact that an integrated health system can have on understanding specific public-health issues.
This new study is remarkable not only in its scope, but also in its long follow-up time and inclusion of only people with symptomatic COVID-19 who had never received any COVID-19 vaccines.
“This data is key to helping us understand the strength and longevity of natural immunity and allows us to compare the effectiveness of a prior infection with mRNA jabs,” said Dr. Amy Compton-Phillips, M.D., Providence’s chief clinical officer. The findings “provide new insight into the length of protection following an initial infection among the population who have never received any COVID-19 jabs and could have important implications for jabs guidelines and public health policy.”
Image Credit: Getty
You were reading: Natural Immunity after catching COVID protected more for a longer time than mRNA vaccines alone