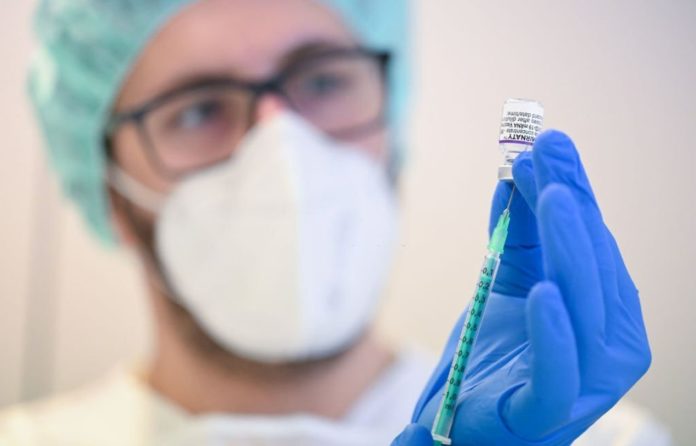
Many immunocompromised people show low responses to COVID vaccines. Patients with IBD who are using anti-TNF therapy may have varied antibody responses to vaccines.
SARS-CoV-2 vaccine immunogenicity is influenced by age, vaccination type, and immunomodulator usage. Other factors, however, have a role in defining the response to the SARS-CoV-2 vaccine that must be investigated.
The current study assumed that the gut microbiota and metabolome, or their functional metabolic output, play an important role in influencing host immune responses. IBD patients, on the other hand, are immunocompromised and have a disrupted gut microbiota and metabolome. It’s probably why they have such a mixed humoral immune response to SARS-CoV-2 immunization.
Furthermore, the composition of the gut microbiota has been linked to immunosuppressive medication responses, such as anti-TNF therapy in IBD. As a result, gut microbial metabolites accurately predict anti-TNF medication response.
The researchers collected serum and fecal samples from adult IBD patients who had been immunized against SARS-CoV-2 with either the BNT162b2 or ChAdOx1 nCoV-19 vaccines. Furthermore, these individuals had been on infliximab for more than 12 weeks. Between the first vaccine dosage and four weeks after getting the vaccine, they collected fecal samples. Similarly, regardless of vaccine timing, the team tested the serum samples of all trial participants at eight-week intervals.
Using an anti-SARS-CoV-2 spike (S) electrochemiluminescence immunoassay, the researchers evaluated the antibody responses of all trial participants after a two-dose immunization regimen. They discovered that only 17 patients (39.5 percent) exhibited serological responses below the geometric mean titer (GMT) of the CLARITY-IBD cohort. The current study’s subjects were all recruited in the CLARITY-IBD study to receive SARS-CoV-2 vaccine. The researchers also used 16S ribosomal ribonucleic acid (rRNA) gene amplicon sequencing and nuclear magnetic resonance (NMR) spectroscopy to examine each patient’s feces. They also employed ultra-high-performance liquid chromatography-mass spectrometry (UHPLC-MS) to profile the bile acids in the feces.
In addition, the researchers used univariable, multivariable, and correlation analyses to find predictors of gut microbial and metabolome responses after vaccination.
Only eight individuals had a history of SARS-CoV-2 infection, as determined by the anti-SARS-CoV-2 nucleocapsid (N) immunoassay, in the trial group of 43 infliximab-treated IBD patients recruited between 25 January and 15 March 2021.
The majority of individuals in a research by Ng and colleagues were healthy, with only 3 percent on immunosuppressive medicine. Furthermore, the majority of trial participants received CoronaVac, an inactivated virus vaccine, while a small percentage received the BNT162b2 vaccine, which is based on messenger RNA. Despite the variations, these studies found that having a parabacteroides was linked to a weaker serological response to SARS-CoV-2 immunization.
The current study also found a link between the abundance of the Bilophila genus and a stronger serological response to SARS-CoV-2 vaccination. Streptococcus, on the other hand, was linked to a lower-than-average serological reaction. In particular, immunization with BNT162b2 resulted in the activation of virus-specific CD4+ T cell responses with a type 1 T helper (TH1) profile; similarly, Bilophila wadsworthensis was linked to an increased pro-inflammatory TH1 response. As a result, the researchers theorized that Bilophila served as a vaccine enhancer in some IBD patients, attracting TH1 cells to produce antibodies against SARS-CoV-2. Notably, those with high and low serological responses to COVID-19 vaccinations showed Bacteroidota and Firmicutes as the major gut flora.
NMR profiling uncovered 36 metabolite characteristics, including five short-chain fatty acids, 11 amino acids, and three respiratory chemicals, whereas UHPLC-MS detected 50 bile acids. Patients with a good serological response to COVID-19 vaccination had higher levels of trimethylamine (TMA), omega-muricholic acid, and ursodeoxycholic acid, according to the univariate analysis.
Patients with a poor COVID-19 vaccination response had higher levels of succinate, phenylalanine, and phenylacetate, according to the researchers. The authors subsequently detected higher fecal PA in IBD patients compared to healthy controls. They also discovered increased succinate levels in Crohn’s disease patients.
Overall, the study found a link between the gut microbiota and IBD patients’ variable serological responses to SARS-CoV-2 immunization. COVID-19 therapies that change the gut microbiota or replenish beneficial metabolites have the potential to effectively repair vaccine-induced immunogenicity. As a result, TMA could aid in reducing the immune response’s weakening caused by anti-TNF.
Image Credit: Getty
You were reading: Your Gut Might be Triggering Poor Response to COVID Vaccines